03 de juny 2015
An open mind on mental health
The social and economic impact of mental illness requires a new approach. Conventional approaches to the disease are insufficient and a broad involvement of different stakeholders is needed. These are the premises that the OECD has drawn in its new report "Fit mind, job fit. From evidence to practice in mental health and work. " While in previous reports had tried to characterize the state of affairs, now he has been concerned to review successful strategies in different countries.
The total costs of mental illness represent around 3.5% of GDP in European countries. Of this, more than half corresponds to indirect and intangible costs. Among them are productivity losses, an aspect difficult to estimate because the phenomenon of "presenteeism" appears. In the case of mental illness, the fact of going to work despite illness is the rule (over 75%) .
The issue presents differential considerations for other diseases, especially its relationship with the job and productivity. There is evidence of less satisfaction, lower quality jobs and lower pay. All contribute to conditions of work under a mental illness represent a tension for the individual and for the company. And of course in the event of unemployment, even more.
Ssome countries have tried to deal with this situation from an interdisciplinary way. That is, strictly avoiding medicalized view of health policy and trying to involve the various actors in the field of business and social environment of the patient.
The OECD recommendations fall into four areas: youth and education, business, social services and employment and healthcare. Of these, I would like to highlight here those related to the firm, being the most neglected at present.
In the field of business, strategies for supporting employees with mental health problems are crucial to achieve a positive development that avoids the end a loss of jobs and a worsening of the disease. The initial issue to consider is the detection of the problem. Somehow, managers and immediate supervisors need to provide a suitable response to the situation and often do not have the knowledge and training needed. The British example known as "Mental Health First Aid program" is a tipping point to keep in mind despite his limited success in small and medium enterprises.
The adoption of risk prevention strategies also seeks to provide tools to improve psychosocial job conditions. To this, a change of perspective in occupational medicine could contribute decisively.In cases of injury, the management of return to work eventually becomes critical for improving the stage of the disease process. To the extent that the long absences are more complex to address, it is precisely these that require attention consistently. The option of gradual return to work and support by colleagues has proven effective in this regard. The search for a negotiated solution brings more satisfactory exit routes for the disease, the conflict. And finally there are the incentive strategies and the legal obligations of employers in this regard. How to address long-term absenteeism it is a challenge in all countries and there is no rècipe for all cases. Must be combined with adequate monitoring incentives to return to the job.The uniqueness of mental illness is that the successful approach is the one that allows redevelopment activities in the labor and social environment properly. To do this, a modern approach requires among other things that the company and its employees are aware of and responsible for a different perspective and fully involved. In this direction, government and business associations should join hands to tackle an issue that so far we thought belonged only to the health system. The relevance of mental health and its impact on the welfare of citizens and their families, requires a timely response.
03 de juny 2016
What's health and wellbeing?
Once again, we do need a comprehensive definition of what is health and wellbeing, and the current issue of PNAS provides us with an interesting approach:
The dominant model of health is a disease-centered Medical Model (MM), which actively ignores many relevant domains. In contrast to the MM, we approach this issue through a Comprehensive Model (CM) of health consistent with the WHO definition, giving statistically equal consideration to multiple health domains, including medical, physical, psychological, functional, and sensory measures. We apply a data-driven latent class analysis (LCA) to model 54 specific health variables from the National Social Life, Health, and Aging Project (NSHAP), a nationally representative sample of US community-dwelling older adults.
Although public health campaigns, such as “Choosing Wisely,” rightly emphasize the need to decrease unnecessary health interventions (52), they still accept the basic health conception of the MM as resting on organ system disease. Instead, the CM instantiates comorbidities and the equal importance of mental health, mobility, and sensory function in health and should inform policy redesign. For example, including assessments of sensory function, mental health, broken bones in middle age, and frailty in annual physician visits would enhance risk management. In addition to policies focused on reducing BMI, greater support for preventing loneliness among isolated older adults would be effective. In place of additional (expensive) new medicines for hypertension, helping older adults find social support through home care services or alternative living arrangements could be developed. In summary, taking a broad definition of health seriously and empirically identifying specific constellations of health and comorbidities in the US population provide a new way of assessing health and risk in older adults living in their homes and thereby, may ultimately inform health policy.And these are the results:
The CM of health with six distinct health classes based on 54 health measures across six dimensions (listed in column 1). The column US population (US Pop.) reports the prevalence in 2005 of each disease or condition in the older US Pop. ages 57–85 y old (definitions and validation are in Fig. S1). Within each health class (columns), the prevalence of a given disease or condition indexes the likelihood that any member of the class has that particular disease [rows; n = 54 health measures ordered by prevalence within each health domain (column 2)] and shares similar constellations of disease and health.
We should reckon on something similar with our data, just to check if it fits with the final goal of measuring health and wellbeing. As you may imagine, there are many implications. If we agree on a comprehensive model of health, then we have to focus on how decisions and priorities should be made.
PS. The return of the big questions. JM Colomer opinion;:
The achievement of a human-made plan depends 1/4 on resources, such as money, education or physical strength; 1/4 on skill and decisions; and 1/2 on unpredictable circumstances, usually called luck. A student asked me how luck can be improved: well, I said, if you keep pursuing your goal with perseverance, the probabilities to get it increase (like if you keep playing the lottery, the probability to get the prize also increases)
26 de novembre 2021
Mental health challenges
From Awareness to Change in Integrated Mental Health, Skills and Work Policies
1 What does a mental health-in-all-policies approach look like?
2 What are current social and labour market outcomes for persons with mental health conditions?
3 How far have we come in implementing integrated mental health, skills and work policies?
4 What are the implications and lessons of the COVID-19 pandemic for integrated mental health, skills and work policy?
A timely OECD report 5 years after the approval of the Recommendation on Integrated Mental Health, Skills and Work Policy. Unfortunately many countries still have to apply them...
13 de febrer 2017
Common challenges and responses to improve healthcare quality
Key messages from the last OECD report on quality:
Systemic changes on where and how health care is delivered will optimise both quality and efficiency
Lesson 1: High-performing health care systems offer primary care as a specialist service that provides comprehensive care to patients with complex needs
Lesson 2: Patient-centred care requires more effective primary and secondary prevention in primary care.
Lesson 3: High-quality mental health care systems require strong health information systems and mental health training in primary care
Lesson 4: New models of shared care are required to promote co-ordination across health and social care systems
Health care systems need to engage patients as active players in improving health care, while modernising the role of health professionals
Lesson 5: A strong patient voice is a priority to keep health care systems focussed on quality when financial pressures are acute
Lesson 6: Measuring what matters to people delivers the outcomes that patients expect
Lesson 7: Health literacy helps drive high-value care
Lesson 8: Continuous professional development and evolving practice maximise the contribution of health professionals
Health care systems need to better employ transparency and incentives as key quality-improvement toolsIt may sound as a dejà-vu, and the difficult part is how, not what to do to improve quality. However if you want to read an article on health care quality comparisons, check this one. Comparing quality is crucial because we are used to compare expenditure without a detailed knowledge of quality achievement. We'll have to follow next reports on the issue.
Lesson 9: High-performing health care systems have strong information infrastructures that are linked to quality-improvement tools
Lesson 10: Linking patient data is a pre-requisite for improving quality across pathways of care
Lesson 11: External evaluation of health care organisation needs to be fed into continuous quality-improvement cycles
Lesson 12: Improving patient safety requires greater effort to collect, analyse and learn from adverse events
20 de març 2023
La salut mental de la població
Measuring Population Mental Health
Ara que es parla tant de la salut mental després de la pandèmia és un bon moment per recordar la importància de mesurar com estem poblacionalment. I això és el que proposa el document que acaba de publicar l'OCDE. Ara bé, l'opció escollida, incorporar preguntes homogènies a les enquestes de salut també té les seves dificultats. Ells mateixos ho assumeixen.
All OECD countries currently measure population mental health, yet use a variety of tools to capture a multitude of outcomes. In order to improve harmonisation, this chapter poses a series of questions that highlight the criteria to be considered when choosing appropriate survey tools. These criteria include statistical quality, practicalities of fieldwork and data analysis. Overall, there is strong evidence supporting the statistical properties of the most commonly used screening tools for the composite scales of mental illhealth and positive mental health. Four concrete tools (the PHQ-4, the WHO- 5 or SWEMWBS, and a question on general mental health status) that capture outcomes across the mental health spectrum are suggested for inclusion in household surveys in addition to already ongoing data collection efforts.
A Catalunya ara mateix estem sense pla director, el 2020 va finalitzar. Aquells que han de preparar el nou poden aprofitar idees d'aquest informe de l'OCDE. Només que mesuréssim correctament ja hi tindríem molt guanyat i molts deixarien de parlar de suposicions.
PD. Cal un pacte nacional? O potser el que cal és més i millor gestió? O simplement ja va sent hora que algú posi fil a l'agulla.
03 de gener 2016
Public health for the world
The book starts with this statement:
“Global Health” is a relatively recent construct, largely replacing and extending concepts embedded in prior terms such as “Tropical Medicine” and “International Health.” We have adopted a working definition of Global Health as “Public Health for the world”. In this view, everyone in the world is the relevant population, and Global Health seeks to prevent and treat the diseases that compromise good health anywhere in the world. A brief review of the origin and evolution of the concept of Global Health may cast light on some of the institutions and impulses still intrinsic to the study of Public Health for the world.That's it. A selections of 18 articles from NEJM (plus intro and conclusions) is presented in the book in order to understand the current change of paradigm:
1. Harvey V. Fineberg and David J. Hunter: A Global View of Health-An Unfolding SeriesThe book is specially appropriate for any health professional and politician. Clearly written and concrete messages, allows the reader to undestand that public health requires a deeper global coordination.
Part I: Global Disease Patterns and Predictions
2. Christopher J.L. Murray and Alan D. Lopez: Measuring the Global Burden of Disease
3. Anthony J. McMichael: Globalization, Climate Change, and Human Health
Part II: Infectious Diseases
4. Anthony S. Fauci and David M. Morens: The Perpetual Challenge of Infectious Diseases
5. Peter Piot and Thomas C. Quinn: Response to the AIDS Pandemic-A Global Health Model
6. Harvey V. Fineberg: Pandemic Preparedness and Response-Lessons from the H1N1 Influenza of 2009
7. Rupa Kanapathipillai, Armand G Sprecher, and Lindsey R Baden: Ebola Virus Disease: Past and Present
8. Gary J. Nabel: Designing Tomorrow's Vaccines
9. Donald R. Hopkins: Disease Eradication
Part III: Non-Communicable Diseases
10. Majid Ezzati and Elio Riboli: Behavioral and Dietary Risk Factors for Noncommunicable Diseases
11. Prabhat Jha and Richard Peto: Global Effects of Smoking, of Quitting, and of Taxing Tobacco
12. David J. Hunter and K. Srinath Reddy: Noncommunicable Diseases
13. Anne E. Becker and Arthur Kleinman: Mental Health and the Global Agenda
14. Robyn Norton and Olive Kobusingye: Injuries
Part IV: Health System Responses
15. Zulfiqar A. Bhutta and Robert E. Black: Global Maternal, Newborn, and Child Health-So Near and Yet So Far
16. Anne Mills: Health Care Systems in Low- and Middle-Income Countries
17. Jennifer Leaning and Debarati Guha-Sapir: Natural Disasters, Armed Conflict, and Public Health
Part V: Global Institutional Responses
18. Julio Frenk and Suerie Moon: Governance Challenges in Global Health
19. Lawrence O. Gostin and Devi Sridhar: Global Health Law
20. Nigel Crisp and Lincoln Chen: Global Supply of Health Professionals
21. David J. Hunter and Harvey V. Fineberg: Convergence to Common Purpose in Global Health
02 de maig 2018
Mental health: the problem and what can be done
I have to recognise it. Mental health is a difficult issue, and all the efforts to decrease its impact on individual and social welfare are not enough by now. The book by Layard and Clark is a useful reference. I had to read it since long time. It says:
Mental illness is the great hidden problem in our societies, so most people are amazed when they hear the scale of it. In the Western world today one in six of all adults suffers from depression or a crippling anxiety disorder. Roughly a third of households currently include someone who is mentally ill.I don't know the exact figure, but I agree with the statement.
Mental illness is not just a problem for those it affects directly. It also imposes huge costs on the rest of society. So the case for tackling the problem is not just humanitarian—it is also a matter of plain economics. Mental health problems diminish work, increase crime, and make additional demands on physical health care.So, what is the cost? The answer is huge. Layard and Clark provide some figures. And in the second part of the book, they review the alternative approaches to the issue. A highly recommended book by one of the greatest economists of our time.
10 d’octubre 2017
Healthcare Quality Lessons
An OECD report provides the lessons on caring for quality, quite general but of interest to dive into each one:
Lesson 1. High-performing health care systems offer primary care as a specialist serviceIt is like a check list, have you done your homework?
that provides comprehensive care to patients with complex needs
Lesson 2. Patient-centred care requires more effective primary and secondary prevention
in primary care
Lesson 3. High-quality mental health care systems require strong health information systems
and mental health training in primary care
Lesson 4. New models of shared care are required to promote co-ordination across health
and social care systems
Lesson 5. A strong patient voice is a priority to keep health care systems focussed
on quality when financial pressures are acute
Lesson 6. Measuring what matters to people delivers the outcomes that patients expect
Lesson 7. Health literacy helps drive high-value care
Lesson 8. Continuous professional development and evolving practice maximise
the contribution of health professionals
Lesson 9. High-performing health care systems have strong information infrastructures
that are linked to quality-improvement tools
Lesson 10. Linking patient data is a pre-requisite for improving quality across pathways
of care
Lesson 11. External evaluation of health care organisation needs to be fed into continuous
quality-improvement cycles
Lesson 12. Improving patient safety requires greater effort to collect, analyse and learn
from adverse events
24 de desembre 2014
Mental Health in the policy agenda
The need for action in mental health is increasingly recognised. Although relevant improvements have been introduced in developed countries, there is a common view that more should be done. Some diseases like depression are at the top of the burden of disease and bring enormous pain and suffering to individuals and their families and communities. An interesting recent report has been released on the topic. This is the infographic:
PS. UK Health Secretary. Keynote address: the political imperatives to address mental health and depression
19 de desembre 2018
At a glance
Every two years OECD publishes this report for the European Union on the state of health. The new one has an interesting thematic chapter on mental health. It says:
According to the latest IHME estimates, more than one in six people across EU countries (17.3%) had a mental health problem in 2016 – that is, nearly 84 million people.And the second thematic chapter is about health expenditure: Strategies to reduce wasteful spending: Turning the lens to hospitals and pharmaceuticals. It says:
The most common mental disorder across EU countries is anxiety disorder, with an estimated 25 million people (or 5.4% of the population) living with anxiety disorders, followed by depressive disorders, which affect over 21 million people (or 4.5% of the
population).An estimated 11 million people across EU countries (2.4%) have drug and alcohol use disorders. Severe mental illnesses such as bipolar disorders affect almost 5 million people (1.0% of the population), while schizophrenic disorders affect another estimated 1.5 million people (0.3%).
For hospitals, reducing or eliminating unnecessary investigations and procedures, many of which expose patients to unnecessary risks without the prospect of clinical benefit, is an obvious target for direct intervention. Expanding the use of day surgery can also be instigated at hospital level. However minimising avoidable admissions, particularly for ambulatory care-sensitive conditions, reducing unnecessary length of stay, and improving discharge processes require broader perspectives. Enhanced primary care services, expanded postacute care facilities, post-discharge care coordination, and in home care services all require health system reforms that cannot be initiated by hospitals alone.
For pharmaceuticals, creating and supporting competitive markets and promoting the uptake of generics and biosimilars can generate substantial savings. That said, reducing waste does not necessarily mean spending less; it may equally be achieved by gaining better value for money from existing expenditure. Both supply and demand side levers offer scope for better value. Using health technology assessment to inform selection, pricing and procurement of new medicines facilitates an understanding of the true opportunity costs of therapies and helps avoid the displacement of high value interventions with ones of lesser value.This is not new. We have already heard the same for years. Therefore, current inertia is supported by strong incentives that prevent change (either in policy or management). This is the key challenge.

05 d’agost 2023
Salut mental
Mad World. The Politics of Mental Health
Introduction
1. Asylums
2. 'Knowing' Mental Health Today
3. Mental Health in a Maddening World
4. Why Work is Sickening
5. Disability / Possibility
6. Diagnosing Diagnosis
7. On Disavowal and Disorder
8. Art for Mental Health
9. Law and Disorder
10. Other Possibilities
Conclusion
11 d’abril 2025
El disseny de sistemes de pagament
A Framework for the Design of Risk-Adjustment Models in Health Care Provider Payment Systems
A partir d'avui aquest blog es trasllada a Substack. Durant unes setmanes serà accessible simultàniament per blogger i per substack. Anoteu l'adreça: econsalut.substack.com
Article resumit amb IA.
Aquest article presenta un marc conceptual integral per al disseny de models d'ajust de risc (RA) en el context de models de pagament prospectiu a proveïdors d'assistència sanitària. L'objectiu és desenvolupar un marc que expliciti les opcions de disseny i les compensacions associades per tal de personalitzar el disseny de l'RA als sistemes de pagament a proveïdors, tenint en compte els objectius i les característiques del context d'interès.
Introducció (1-3): Durant les últimes dècades, els reguladors i els responsables polítics de la salut han fet esforços per millorar l'eficiència de la prestació d'assistència sanitària mitjançant la reforma dels sistemes de pagament a proveïdors. Específicament, l'eficiència s'ha perseguit mitjançant la introducció d'elements prospectius en els models de pagament, donant lloc a diversos Models de Pagament Alternatius (MPA) com els acords de qualitat alternatius i els pagaments agrupats. Aquests MPA tenen com a objectiu incentivar l'eficiència traslladant (part de) la responsabilitat financera dels pagadors als proveïdors. Una característica típica dels pagaments prospectius a proveïdors és que es basen en un "nivell de despesa normatiu" per a la prestació d'un conjunt predefinit de serveis a una determinada població de pacients. El nivell de despesa normatiu es refereix al nivell de despesa que "hauria de ser" depenent de la població de pacients d'un proveïdor, en lloc de la despesa observada. Un element clau en la determinació dels nivells de despesa normatius és la correcció de les diferències sistemàtiques en les necessitats d'assistència sanitària de les poblacions de pacients dels proveïdors, comunament coneguda com a ajust de risc (RA). L'RA és crucial per garantir un terreny de joc igualitari per als proveïdors i per evitar incentius per a comportaments no desitjats, com la selecció de riscos.
Nova Contribució (8-10): Tot i les contribucions conceptuals existents sobre el disseny de l'RA, actualment no hi ha un marc integral per adaptar el disseny de l'RA al pagament de proveïdors i a les característiques essencials del context. Aquest article desenvolupa aquest marc sintetitzant, ampliant i aplicant coneixements de la literatura existent. La metodologia va incloure una revisió de la literatura combinada amb consultes a experts en el camp de l'RA i els sistemes de pagament. La informació recopilada es va sintetitzar per desenvolupar el marc, del qual van sorgir tres criteris per al disseny de models d'RA i es van agrupar les opcions i les compensacions en dues dimensions principals: (a) la tria dels ajustadors de risc i (b) la tria de les ponderacions de pagament.
Definicions de Conceptes Clau (11-13): Els models de pagament prospectiu i els MPA traslladen la responsabilitat financera dels pagadors als proveïdors per tal d'incentivar el control de costos i l'eficiència. Qualsevol trasllat de responsabilitat financera requereix que el pagador determini el nivell de despesa normatiu, que reflecteix el nivell de despesa apropiat donades les necessitats d'assistència sanitària d'una població i els objectius dels MPA. El nivell de despesa normatiu no fa referència necessàriament al nivell de despesa absolut o òptim, sinó al nivell considerat apropiat donat el nivell/objectius d'eficiència perseguits pel MPA.
Fonts de Variació de la Despesa i el Paper de l'RA i la Mancomunació de Riscos (14-19): Quan s'estableixen nivells de despesa normatius, és important considerar tres fonts de variació de la despesa: (a) variació sistemàtica impulsada per factors fora del control dels proveïdors (variables C o "factors de compensació"), (b) variació sistemàtica impulsada per factors que els proveïdors poden influir (variables R o "factors de responsabilitat"), i (c) variació aleatòria. Per evitar que els proveïdors assumeixin riscos excessius que no poden influir, els MPA solen aplicar alguna forma de mancomunació de riscos. L'RA prospectiu s'utilitza per compensar la variació de la despesa deguda a les variables C. La naturalesa i el grau en què s'ha de compensar la variació de la despesa resultant de les variables C forma el punt de partida d'un model d'RA.
Tres Criteris per al Disseny de Models d'RA (19-26): L'objectiu general de l'RA en els MPA és compensar els proveïdors per la variació de la despesa deguda a les variables C, alhora que els manté responsables de la variació de la despesa deguda a les variables R. Això implica dos criteris clau: (a) compensació adequada per a les variables C i (b) cap compensació per a les variables R. Un tercer criteri important és la viabilitat.
- Criteri 1: Compensació Adequada per a les Variables C (20-26): Per evitar problemes de selecció, l'RA hauria de compensar adequadament les variables C que són rellevants a la llum de les possibles accions de selecció de riscos per part dels proveïdors (atraure/dissuadir pacients sans/no sans). També hauria de compensar les variables C que varien entre les poblacions de proveïdors per evitar la participació selectiva en el MPA.
- Criteri 2: Cap Compensació per a les Variables R (26-29): Per evitar ineficiències, l'RA no hauria de compensar les variables R. La compensació per la variació de la despesa de les variables R pot donar lloc a problemes d'eficiència, com la perpetuació de les ineficiències existents ("biaix d'status quo") i la creació d'incentius per a noves ineficiències (reducció dels incentius per al control de volum i preu, codificació ascendent).
- Criteri 3: Viabilitat (29-30): Un tercer criteri crucial és la viabilitat, que inclou la disponibilitat de dades i l'acceptació per part de totes les parts interessades (pacients, proveïdors, pagadors, reguladors).
Un Marc per al Disseny de Models d'RA (30-31): Aquest marc distingeix entre preguntes de disseny, opcions associades i consideracions i compensacions clau pel que fa a (a) la tria dels ajustadors de risc i (b) la tria de les ponderacions de pagament.
La Tria dels Ajustadors de Risc (31-47): Aquesta secció aborda tres preguntes principals de disseny:
- Quin tipus d'informació es basa els ajustadors de risc? (32-38): Les opcions inclouen informació demogràfica, socioeconòmica, subjectiva (de salut), diagnòstica, d'utilització, clínica, de despesa (retardada) i del costat de l'oferta. L'ús d'informació endògena (diagnòstics, utilització, despesa) és altament predictiu de la despesa de tipus C, però pot perpetuar ineficiències i introduir nous incentius perversos per al volum i el preu. L'ús d'informació exògena (demogràfica, socioeconòmica) no manté ni introdueix incentius perversos relacionats amb el volum o el preu, però el seu poder predictiu és generalment baix.
- A quin període de temps (període base) pertany la informació? (38-45): Es pot distingir entre ajustadors concurrrents i prospectius. Els efectes d'incentiu relatius d'aquestes opcions no estan clars a priori.
- Com dissenyar els ajustadors de risc? (46-47): Això inclou l'especificació de l'escala de mesura, l'operacionalització dels ajustadors (considerant condicions, jerarquies, restriccions) i les interaccions entre ajustadors.
La Tria de les Ponderacions de Pagament (48-60): Per trobar ponderacions de pagament apropiades, els responsables de la presa de decisions s'enfronten a tres decisions principals de disseny:
- Quina mostra d'estimació? (49-52): Es requereix una mostra d'estimació representativa de la població d'interès i dels nivells de despesa normatius. En la pràctica, sovint s'utilitzen dades històriques i poblacions de pacients similars.
- Quines intervencions de dades? (52-58): Quan la mostra d'estimació no és representativa, s'han de considerar intervencions de dades sobre la població de pacients i/o les dades de despesa per millorar la coincidència amb la població d'interès i el nivell de despesa normatiu. Això pot incloure correccions per biaixos i inequitats.
- Com derivar les ponderacions de pagament? (59-60): Això implica decidir quins ajustadors de risc incloure (considerant el biaix de la variable omesa) i quin criteri d'optimització utilitzar per estimar aquestes ponderacions. Les opcions van des de criteris d'optimització estàndard (OLS, GLM) fins a criteris personalitzats (regressió restringida, aprenentatge automàtic).
La Interconnexió Entre les Opcions de Disseny per als Ajustadors de Risc i les Ponderacions de Pagament (61-62): Les decisions de disseny dins i entre aquests dos temes estan altament interrelacionades. Per exemple, la tria de la informació en què es basen els ajustadors de risc afectarà la seva especificació i operacionalització. De la mateixa manera, les decisions sobre com es deriven les ponderacions de pagament depenen tant de la tria dels ajustadors de risc com de la tria de la mostra d'estimació (modificada).
Discussió (63-68): No hi ha un enfocament únic per al disseny de models d'RA, i el disseny adequat pot variar segons la configuració i les evolucions al llarg del temps. És crucial la decisió normativa sobre quines variables es consideren C i quines R. L'abast de la preocupació pels possibles incentius de selecció i control de costos pot variar segons el context. Les consideracions de viabilitat, com la disponibilitat de dades i l'acceptació de les parts interessades, també són importants.
Consideracions Més Amplies per al Disseny de l'RA en el Finançament de l'Assistència Sanitària (69-70): Tot i que aquest article se centra en el pagament a proveïdors, el marc proposat també podria beneficiar altres reformes de finançament, com les iniciatives de participació del consumidor, tot i que es necessita més recerca.
Conclusió (71): El disseny de models d'RA per a sistemes de pagament prospectiu a proveïdors és un exercici complex que requereix una consideració explícita de moltes preguntes, opcions i compensacions difícils. El procés de disseny ha de guiar-se per tres criteris clau: compensació adequada de les variables C, cap compensació de les variables R i viabilitat. Les diverses preguntes i opcions de disseny es poden classificar en la tria dels ajustadors de risc i la tria de les ponderacions de pagament. Es necessita més recerca per donar suport a les decisions normatives sobre les variables C i R, així com per desenvolupar mètriques d'avaluació integrals per a la valoració dels efectes dels incentius.
Referències
A continuació es mostren les referències citades en les fonts:
- Adams Dudley, R., Medlin, C. A., Hammann, L. B., Cisternas, M. G., Brand, R., Rennie, D. J., & Luft, H. S. (2003). The best of both worlds? Potential of hybrid prospective/concurrent risk adjustment. Medical Care, 41(1), 56–69.
- American Medical Association. (2019). Improving Risk adjustment in alternative payment models.
- Andersen, R., & Newman, J. F. (2005). Societal and individual determinants of medical care utilization in the United States. The Milbank Memorial Fund Quarterly. Health and Society, 83(4), 1468-0009.2005.00428.x.
- Anderson, G. F., & Weller, W. E. (1999). Methods of reducing the financial risk of physicians under capitation. Archives of Family Medicine, 8(2), 149–155.
- Anthun, K. S. (2021). Predicting diagnostic coding in hospitals: Individual level effects of price incentives. International Journal of Health Economics and Management, 22(2), 129–146.
- Arrow, K. J. (2004). Uncertainty and the welfare economics of medical care. Bulletin of the World Health Organization, 82(2), 141–149.
- Ash, A. S., & Ellis, R. P. (2012). Risk-adjusted payment and per-formance assessment for primary care. Medical Care, 50(8), 643–653.
- Ash, A. S., Mick, E. O., Ellis, R. P., Kiefe, C. I., Allison, J. J., & Clark, M. A. (2017). Social determinants of health in managed care payment formulas. JAMA Internal Medicine, 177(10), 1424–1430.
- Bäuml, M. (2021). How do hospitals respond to cross price incen-tives inherent in diagnosis-related groups systems? The impor-tance of substitution in the market for sepsis conditions. Health Economics, 30(4), 711–728.
- Bergquist, S. L., Layton, T. J., McGuire, T. G., & Rose, S., & National Bureau of Economic Research. (2018). Intervening on the data to improve the performance of health plan pay-ment methods (Ser. NBER working paper series, no. w24491). National Bureau of Economic Research.
- Brown, J., Duggan, M., Kuziemko, I., & Woolston, W. (2014). How does risk selection respond to risk adjustment? New evi-dence from the Medicare Advantage Program. The American Economic Review, 104(10), 3335–3364.
- Buchner, F., Wasem, J., & Schillo, S. (2017). Regression trees iden-tify relevant interactions: Can this improve the predictive per-formance of risk adjustment? Health Economics, 26(1), 74–85.
- Cattel, D., Eijkenaar, F., & Schut, F. T. (2020). Value-based pro-vider payment: Towards a theoretically preferred design. Health Economics, Policy and Law, 15(1), 94–112.
- Chang, H.-Y., Lee, W.-C., & Weiner, J. P. (2010). Comparison of alternative risk adjustment measures for predictive modeling: High risk patient case finding using Taiwan’s national health insurance claims. BMC Health Services Research, 10, 343– 343. https://doi.org/10.1186/1472-6963-10-343.
- Chernew, M. E., Mechanic, R. E., Landon, B. E., & Safran, D. G. (2011). Private-payer innovation in Massachusetts: The “alter-native quality contract.” Health Affairs, 30(1), 51–61.
- Chien, A. T., Newhouse, J. P., Iezzoni, L. I., Petty, C. R., Normand, S.-L. T., & Schuster, M. A. (2017). Socioeconomic background and commercial health plan spending. Pediatrics, 140(5).
- Constantinou, P., Tuppin, P., Gastaldi-Ménager, C., & Pelletier-Fleury, N. (2022). Defining a risk-adjustment formula for the introduction of population-based payments for primary care in France. Health Policy, 126(9), 915–924.
- Dafny, L. S. (2005). How do hospitals respond to price changes? The American Economic Review, 95(5), 1525–1547.
- Douven, R., McGuire, T. G., & McWilliams, J. M. (2015). Avoiding unintended incentives in ACO payment models. Health Affairs, 34(1), 143–149.
- Douven, R., Remmerswaal, M., & Mosca, I. (2015). Unintended effects of reimbursement schedules in mental health care. Journal of Health Economics, 42, 139–150.
- Dowd, B. E., Huang, T-y, & McDonald, T. (2021). Tiered cost-sharing for primary care gatekeeper clinics. American
- Duan, N., Manning, W. G., Morris, C. N., & Newhouse, J. P. (1983). A comparison of alternative models for the demand for medical care. Journal of Business & Economic Statistics, 1(2), 115–126.
- Durfey, S. N. M., Kind, A. J. H., Gutman, R., Monteiro, K., Buckingham, W. R., DuGoff, E. H., & Trivedi, A. N. (2018). Impact of risk adjustment for socioeconomic status on Medicare advantage plan quality rankings. Health Affairs, 37(7), 1065–1072.
- Eijkenaar, F., van Vliet, R. C. J. A., & van Kleef, R. C. (2018). Diagnosis-based cost groups in the Dutch risk-equalization model: Effects of clustering diagnoses and of allowing patients to be classified into multiple risk-classes. Medical Care, 56(1), 91–96.
- Einav, L., Finkelstein, A., Ji, Y., & Mahoney, N. (2022). Voluntary regulation: Evidence from Medicare payment reform. The Quarterly Journal of Economics, 137(1), 565–618.
- Ellis, R. P. (1998). Creaming, skimping and dumping: Provider competition on the intensive and extensive margins. Journal of Health Economics, 17(5), 537–555.
- Ellis, R. P., Martins, B., & Rose, S. (2018). Risk adjustment for health plan payment. In T. G. McGuire & R. C. van Kleef (Eds.), Risk adjustment, risk sharing and premium regu-lation in health insurance markets: Theory and practice (pp. 55–104). Elsevier.
- Epstein, A. M., & Cumella, E. J. (1988). Capitation payment: Using predictors of medical utilization to adjust rates. Health Care Financing Review, 10(1), 51–69.
- García-Goñi, M., Ibern, P., & Inoriza, J. M. (2009). Hybrid risk adjustment for pharmaceutical benefits. The European Journal of Health Economics, 10(3), 299–308.
- Geruso, M., & Layton, T. (2020). Upcoding: Evidence from Medicare on squishy risk adjustment. Journal of Political Economy, 128(3), 984–1026.
- Geruso, M., & McGuire, T. G. (2016). Tradeoffs in the design of health plan payment systems: Fit, power and balance. Journal of Health Economics, 47, 1–19.
- Gilmer, T., Kronick, R., Fishman, P., & Ganiats, T. G. (2001). The Medicaid Rx model: Pharmacy-based risk adjustment for pub-lic programs. Medical Care, 39(11), 1188–1202.
- Glazer, J., & McGuire, T. G. (2002). Setting health plan premiums to ensure efficient quality in health care: Minimum variance optimal risk adjustment. Journal of Public Economics, 84(2), 153–173.
- Gravelle, H., Sutton, M., Morris, S., Windmeijer, F., Leyland, A., Dibben, C., & Muirhead, M. (2003). Modelling supply and demand influences on the use of health care: Implications for deriving a needs-based capitation formula. Health Economics, 12(12), 985–1004.
- Hayen, A. P., van den Berg, M. J., Meijboom, B. R., Struijs, J. N., & Westert, G. P. (2015). Incorporating shared savings pro-grams into primary care: From theory to practice. BMC Health Services Research, 15, Article 580.
- Heckman, J. J., & Honoré, B. E. (1990). The empirical content of the Roy model. Econometrica, 58(5), 1121–1149.
- Hildebrandt, H., Hermann, C., Knittel, R., Richter-Reichhelm, M., Siegel, A., & Witzenrath, W. S. (2010). Gesundes Kinzigtal Integrated Care: Improving population health by a shared health
- Hollenbeak, C. S. (2005). Functional form and risk adjustment of hospital costs: Bayesian analysis of a Box-Cox random coef-ficients model. Statistics in Medicine, 24(19), 3005–3018. https://doi.org/10.1002/sim.2172.
- Horn, S. D., Horn, R. A., & Sharkey, P. D. (1984). The severity of illness index as a severity adjustment to diagnosis-related groups. Health Care Financing Review, 1984, 33–45.
- Hughes, J. S., Averill, R. F., Eisenhandler, J., Goldfield, N. I., Muldoon, J., Neff, J. M., & Gay, J. C. (2004). Clinical risk groups (CRGs): A classification system for risk-adjusted capitation- based payment and health care management. Medical Care, 42(1), 81–90.
- Humbyrd, C. J., Hutzler, L., & DeCamp, M. (2019). The ethics of success in bundled payments: Respect, beneficence, and social justice concerns. American Journal of Medical Quality, 34(2), 202–204.
- Jha, A. (2014) The Health Care Blog. https://thehealthcareblog. com/blog/2014/09/29/changing-my-mind-on-ses-adjustment/
- Iezzoni, L. I. (2012). Risk adjustment for measuring health care outcomes (3rd ed.). Health Administration Press.
- Iommi, M., Bergquist, S., Fiorentini, G., & Paolucci, F. (2022). Comparing risk adjustment estimation methods under data availability constraints. Health Economics, 31(7), 1368–1380.
- Isaksson, D., Blomqvist, P., Pingel, R., & Winblad, U. (2018). Risk selection in primary care: A cross-sectional fixed effect analysis of Swedish individual data. BMJ Open, 8(10), Article e020402.
- Jones, A. (2010). Models for health care [Working papers]. HEDG, c/o Department of Economics, University of York, Health, Econometrics and Data Group (HEDG).
- Kapur, K., Tseng, C. W., Rastegar, A., Carter, G. M., & Keeler, E. (2003). Medicare calibration of the clinically detailed risk information system for cost. Health Care Financing Review, 25(1), 37–54.
- Lamers, L. M. (1998). Risk-adjusted capitation payments: Developing a diagnostic cost groups classification for the Dutch situation. Health Policy, 45(1), 15–32.
- Lamers, L. M. (1999). Pharmacy costs groups. Medical Care, 37(8), 824–830.
- Lamers, L. M., & van Vliet, R. C. J. A. (2003). Health-based risk adjustment; Improving the pharmacy-based cost group model to reduce gaming possibilities. European Journal of Health Economics, 4(2), 107–114.
- Layton, T. J., McGuire, T. G., & van Kleef, R. C. (2018). Deriving risk adjustment payment weights to maximize efficiency of health insurance markets. Journal of Health Economics, 61, 93–110.
- Lemke, K. W., Pham, K., Ravert, D. M., & Weiner, J. P. (2020). A revised classification algorithm for assessing emergency department visit severity of populations. American Journal of Managed Care, 26(3), 119–125. https://doi.org/10.37765/ ajmc.2020.42636.
- Levy, S., Bagley, N., & Rajkumar, R. (2018). Reform at risk— mandating participation in alternative payment plans. The New England Journal of Medicine, 378(18), 1663–1665.
- Liao, J. M., Pauly, M. V., & Navathe, A. S. (2020). When should Medicare mandate participation in alternative payment mod-els? Health Affairs, 39(2), 305–309.
- Martinussen, P. E., & Hagen, T. P. (2009). Reimbursement sys-tems, organisational forms and patient selection: Evidence from day surgery in Norway. Health Economics, Policy, and Law, 4(Pt. 2), 139–158.
- McGuire, T. G. (2000). Physician agency. In A. J. Culter & J. P. Newhouse (Eds.), Handbook of health economics (1st ed., Vol. Volume 1a, Handbooks in economics, p. 17). Elsevier.
- McGuire, T. G. (2011) Physician agency and payment for primary medical care. In S. Glied & P. C. Smith (Eds), Chapter 9: The Oxford handbook of health economics (online ed., pp. 462– 528). Oxford Academic.
- McWilliams, J. M., Hatfield, L. A., Landon, B. E., Hamed, P., & Chernew, M. E. (2018). Medicare Spending after 3 years of the Medicare shared savings program. The New England Journal of Medicine, 379(12), 1139–1149.
- McWilliams, J. M., Weinreb, G., Ding, L., Ndumele, C. D., & Wallace, J. (2023). Risk adjustment and promoting health equity in population-based payment: Concepts and evidence: Study examines accuracy of risk adjustment and payments in promoting health equity. Health Affairs, 42(1), 105–114.
- Newhouse, J. P. (1994). Patients at risk: Health reform and risk adjustment. Health Affairs, 13(1), 132–146.
- Newhouse, J. P., Price, M., McWilliams, J. M., Hsu, J., & McGuire, T. G. (2015). How much favorable selection is left in Medicare advantage? American Journal of Health Economics, 1(1), 1– 26. https://doi.org/10.1162/ajhe_a_00001.
- Politzer, E. (2024). Utilization thresholds in risk adjustment sys-tems. American Journal of Health Economics, 10(3), 470–503.
- Pope, G. C., Kautter, J., Ellis, R. P., Ash, A. S., Ayanian, J. Z., Lezzoni, L. I., Ingber, M. J., Levy, J. M., & Robst, J. (2004). Risk adjustment of Medicare capitation payments using the CMS-HCC model. Health Care Financing Review, 25(4), 119–141.
- Pope, G. C., Kautter, J., Ingber, M. J., Freeman, S., Sekar, R., & Newhart, C. (2011). Evaluation of the CMS-HCC Risk Adjustment Model [Prepared by RTI]. Centers for Medicare & Medicaid Services, Medicare Plan Payment Group, Division of Risk Adjustment and Payment Policy.
- Porter, M. E., & Kaplan, M. S. (2016). How to pay for health care? Harvard Business Review, 94(7/8), 88–102.
- Robinson, J. C., Whaley, C., Brown, T. T., & Dhruva, S. S. (2020). Physician and patient adjustment to reference pricing for drugs. JAMA Network Open, 3(2), Article e1920544.
- Rose, S. (2016). A machine learning framework for plan payment risk adjustment. Health Services Research, 51(6), 2358–2237.
- Rose, S., Zaslavsky, A. M., & McWilliams, J. M. (2016). Variation in accountable care organization spending and sensitivity to risk adjustment: Implications for benchmarking. Health Affairs, 35(3), 440–448.
- Schokkaert, E., & Van de Voorde, C. (2004). Risk selection and the specification of the conventional risk adjustment formula. Journal of Health Economics, 23, 1237–1259.
- Schokkaert, E., & Van de Voorde, C. (2006). Incentives for risk selection and omitted variables in the risk adjustment formula. Annales d’economie et de Statistique, 83-84, 327–352.
- Struijs, J. N., de Vries, E. F., Baan, C. A., van Gils, P. F., & Rosenthal, M. B. (2020). Bundled-payment models around the world: How they work and what their impact has been [Issue brief]. The Commonwealth Fund.
- van Barneveld, E. M., Lamers, L. M., van Vliet René, C. J. A., & van de Ven, W. P. M. M. (2001). Risk sharing as a supplement to imperfect capitation: A tradeoff between selection and effi-ciency. Journal of Health Economics, 20(2), 147–168.
- van de Ven, W. P. M. M., & Ellis, R. P. (2000). Risk adjustment in competitive health plan markets. In A. J. Collyer & J. P. Newhouse (Eds.), Handbook of health economics (pp. 1003– 1092). Elsevier Science.
- van de Ven, W. P. M. M., & van Vliet, R. C. J. A. (1992). How can we prevent cream skimming in a competitive health insur-ance market? The great challenge for the ‘90’s. In P. Zweifel & H. E. French (Eds.), Health economics worldwide (pp. 23–46). Kluwer Academic Publishers.
- van Kleef, R. C., Eijkenaar, F., van Vliet René, C. J. A., & Nielen, M. M. J. (2020). Exploiting incomplete information in risk adjustment using constrained regression. American Journal of Health Economics, 6(4), 477–497.
- van Kleef, R. C., McGuire, T. G., van Vliet René, C. J. A., & van de Ven, W. P. P. M. (2017). Improving risk equalization with constrained regression. The European Journal of Health Economics: Health Economics in Prevention and Care, 18(9), 1137–1156.
- van Kleef, R. C., & Reuser, M. (2021). How the covid-19 pan-demic can distort risk adjustment of health plan payment. The European Journal of Health Economics, 22(7), 1005–1016.
- van Kleef, R. C., & van Vliet René, C. J. A. (2012). Improving risk equalization using multiple-year high cost as a health indicator. Medical Care, 50(2), 140–144.
- Veen, S. H. C. M., Kleef, R. C., Ven, W. P. M. M., & Vliet, R. C. J. A. (2018). Exploring the predictive power of interaction terms in a sophisticated risk equalization model using regres-sion trees. Health Economics, 27(2), 12.
- Vermaas, A. (2006). Agency, managed care and financial-risk sharing in general medical practice [Dissertation]. Erasmus Universiteit.
- Werbeck, A., Wübker, A., & Ziebarth, N. R. (2021). Cream skim-ming by health care providers and inequality in health care access: Evidence from a randomized field experiment. Journal of Economic Behavior and Organization, 188, 1325–1350.
- Withagen-Koster, A. A., van Kleef, R. C., & Eijkenaar, F. (2020). Incorporating self-reported health measures in risk equaliza-tion through constrained regression. The European Journal of Health Economics, 21(4), 513–528.
04 de febrer 2024
La carpeta del ministre de sanitat
Health Ministerial Meeting. Better policies for resilient health systems
Cada any al mateix temps que hi ha la trobada de Davos, es reuneixen el ministres de salut de l'OCDE. I si algun dia us nomenen ministre, us tocarà anar-hi i us donaran una carpeta amb l'informe que adjunto que repassa els grans temes del moment. Estudieu-lo amb deteniment. Aquest any aquestes eren les qüestions:
Working lunch on climate change and health
1 The future of digital health after COVID-19
2 Bolstering public health: Healthy populations for more resilient health systems
3 Strengthening mental health resilience
4 The future of pharmaceutical policy
5 Investing in resilience: The health and social care workforce
Primer de tot un dinar, per parlar del temps (vull dir del clima i la salut) i després temes coneguts dels que darrerament han sortit informes específics i que ja hem explicat en aquest blog.
Aquest gràfic resumeix la petjada de l'assistència sanitària en el clima, i mireu quins Estats tenen la taxa d'emisions més alta:
Crec que no se'n parla prou. I després, trobareu aquest altre gràfic sobre els preus dels nous medicaments (als USA):Per tal que ens fem la idea del que ve, i del que hem parlat repetidament.
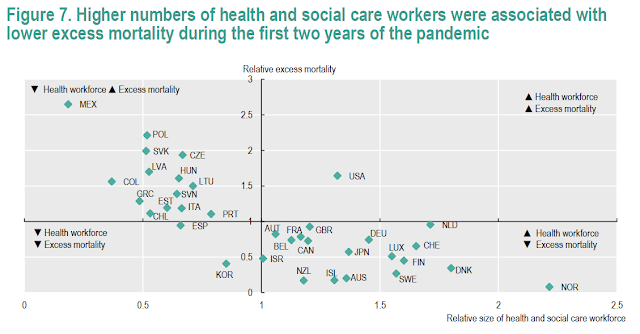
I finalment la relació entre el nombre de treballadors socials i sanitaris i l'excés de mortalitat a la pandèmia:
Jutgeu vosaltres mateixos, la gràfica ho diu tot. Mireu on es troba cada país, i qui hi ha al quadrant inferior de la dreta, i qui no hi és.
PS . I aquesta era l'agenda. Catalunya no hi era a la reunió, la Gemma Galdón si, i què hi feia? (parlava, de què? no ho sé). Si voleu veure-ho, ho trobareu aquí.
PS. I aquestes són les conclusions, on diuen al que es comprometen (ben poca cosa):
WE COMMIT to:
●improve the performance, people-centredness, and resilience of our health systems, through mutual learning and continuous improvement;
●strengthen trust in the use of AI and digital technologies, including improving health data governance globally by strengthening the dissemination and uptake, in particular in other international fora, of the OECD Recommendation on Health Data Governance; and improving health literacy; and
●use artificial intelligence in health systems in a way that is responsible, people-centred and sensitive to ethical concerns; and identify areas where health-specific regulation may be needed.
12 de maig 2021
Health behaviors and behavior change
Behavioral Economics and Public Health
Health behaviors and practices constitute the foundation of good physical and mental health. The leading contributors to the global burden of disease include tobacco smoking, low-quality diets, alcohol abuse, physical inactivity, and obesity. Accordingly, encouraging people to adopt—and maintain—healthy behaviors is a major objective of public health.
Today I recommend this book and this is what you'll find inside:
Chapter 1: An Introduction to Behavioral Economics and Public Health. Christina A. Roberto and Ichiro Kawachi
Chapter 2: Intertemporal Choices for Health. Justin S. White and William H. Dow
Chapter 3: Maintenance of Healthy Behaviors: Forming and Changing Habits. Dennis Rünger and Wendy Wood
Chapter 4: Emotions and Health Decision-Making: Extending the Appraisal Tendency Framework to Improve Health and Health Care. Rebecca Ferrer, William Klein, Jennifer Lerner, Valerie Reyna, and Dacher Keltner
Chapter 5: Social Norms, Beliefs, and Health. Brent McFerran
Chapter 6: Communicating for action: the importance of memorability and actionability. Jason Riis and Rebecca K. Ratner
Chapter 7:Nudging Individuals Toward Healthier Food Choices with the 4Ps Framework for Behavior Change. Zoë Chance, Ravi Dhar, Michelle Hatzis, and Kim Huskey
Chapter 8: Incentivizing Health Behaviors. Kristina Lewis and Jason Block
Chapter 9: Slim By Design: Moving from Can't to CAN.Brian Wansink
Chapter 10: Applying Behavioural Economics in a Health Policy Context: Dispatches from the front lines. Michael Sanders and Michael Hallsworth
Chapter 11: From Choice Architecture to Policy Infrastructure: Multi-Level Theory and the Political Economy of Health Behaviors. Frederick J. Zimmerman
05 de juny 2014
Mental health case-mix measurement
If there is an area where case-mix measurement has been difficult to tackle it is mental health. After all these years, there are several options, but they need an assessment and adaptation to the context of care.
Fortunately there is an excellent review that can be used as starting point. A York University paper commissioned by UK Health Department that tries to compare a UK specific system and its potential application for budgeting and payment:
The Care Pathways and Packages Clusters classification system addresses both clinical and nonclinical needs. Care pathways have been mapped, although the degree of clinical consensus for these is unclear. Nonetheless, they offer a starting point from which to develop consensus. The English approach will require a more systematic approach to data collection and reporting. This offers an opportunity to collect additional data on resource use and process or outcome measures that can help evaluate quality and cost-effectiveness, and so inform the debate on what constitutes best clinical practice. Over time, it may be possible to introduce Pay-for-Performance (P4P) elements into the system, so that good practice is appropriately rewarded. However, P4P using a target based approach can encourage ‘tunnel vision’, in which non-incentivised activity is displaced and would counteract the holistic approach embodied in the Care Pathways and Packages ClustersIs there anybody thinking about this issue nearby?
04 d’agost 2021
Reordering our society is possible
What We Owe Each Other.A New Social Contract for a Better Society
A thought -provoking book. Chapter 5 is devoted to Health:
Being healthy is the most important determinant of our wellbeing. Physical and mental health (subjective well-being as it is called in the academic research) rank at the top of every major study of happiness across the world. Ultimately, this is why every society aspires to provide health care for its population. And because the costs of providing health care are reduced when a large population pools its resources, and because a healthy labour force is also good for the economy, the social contract in every society includes health care in some form or another.
The great issues:
- Defining a Minimum for Universal Health Care
- How Should Health Care Be Provided?
- Health Spending Is Only Going Up
- A More Digital Future for Health
- Individual and Social Responsibilities – Where Is the Balance?
We owe each other more. A more generous and inclusive social contract would recognise our interdependencies, provide minimum protections to all, share some risks collectively and ask everyone to contribute as much as they can for as long as they can. This is not about increasing the welfare state, but about investing in people and building a new system of risk sharing to increase overall well-being. Change will come inevitably because the forces of technology, demography and environmental pressures will drive it. The question is whether we prepare for that change or continue to allow our societies to be buffeted by these powerful forces, as we have in recent decades. This book lays out the challenges we face and provides a menu of alternatives for a better social contract around families, education, health, work, old age and between the generations. It is not a blueprint, but it provides a direction of travel that is economically feasible. Nor is it a fixed menu – countries may choose to implement some elements and not others depending on their values and preferences.
25 de novembre 2022
Wellbeing as a top priority
Why not focus directly on increasing measured human happiness? Why not try to improve people’s overall quality of life, as it is subjectively seen by citizens themselves?
Contents:
Introduction: Making Wellbeing Policies Effective
Timothy Besley & Irene Bucelli
Wellbeing as the Goal of Policy
Richard Layard
Accounting for Consequences and Claims in Policy
Paul Dolan
Weighing the Costs and Benefits of Public Policy: On the Dangers of Single Metric Accounting
Johanna Thoma
Wellbeing in Public Policy: Contributions Based on Sen’s Capability Approach
Paul Anand
Incorporating Wellbeing and Mental Health Research to Improve Pandemic Response
Michael Daly & Liam Delaney
COVID-19 and Mental Health and Wellbeing Research: Informing Targeted, Integrated, and Long-Term Responses to Health Emergencies
Annette Bauer
Health, Wellbeing, and Democratic Citizenship: A Review and Research Agenda
Christopher J. Anderson et al.
Health and Disability Gaps in Political Engagement: A Short Review
Mikko Mattila
28 de juliol 2012
Una recessió saludable?
Els animals s'adapten al medi, els humans també. I si el medi esdevé hostil, aleshores prenem precaucions. Si aquesta recessió ha portat a canviar els comportaments individuals cap a un estil de vida més saludable aquí aprop encara no ho sabem. A Islàndia en canvi ja ho han confirmat. Les conclusions d'un article de NBER són les següents:
The 2008 economic crisis in Iceland led to reductions in all health-compromisingAixí doncs semblaria que a Islàndia la recessió és força bona per la salut. En qualsevol cas, això cal agafar-ho amb pinces i no es pot generalitzar ni extendre temporalment més enllà de l'anàlisi feta. Més aviat diria que cal que ens preguntem si cal una recessió per arribar a comportaments saludables o potser ja va sent hora de fer-ho al marge de l'evolució de l'economia.
behaviors examined—smoking; heavy drinking; consumption of sugared soft drinks, sweets, and fast food; and indoor tanning. It also led to reductions in certain health-promoting behaviors but increased others. Specifically, the crisis reduced consumption of fruits and vegetables but
increased consumption of fish oil and getting the recommended amount of sleep. Generally, the
effects of the crisis on health-compromising behaviors were stronger for the working-age
population than for the adult population overall.
Changes in hours of work, real household income, wealth, and mental health explained
some of the effects on health-compromising behaviors, ranging from 9% for smoking to 42% for heavy drinking. For health-promoting behaviors, these factors reduced the effects of the crisis only for fish oil and vitamins/supplements, by about one third. We inferred that broad-based factors—such as prices, which increased over 27% in Iceland between 2007 and 2009—played a large role in the effects of the crisis on health behaviors. We exploited our ability to isolate behavioral changes that are likely due, at least in large part, to price changes, to compute participation elasticities for the various goods. We found inelastic responses to price changes for alcohol and sugared soft drinks and elastic responses for smoking, sweets, indoor tanning, and fast food. Health-promoting behaviors revealed less price sensitivity overall compared to health compromising behaviors.
M'ha agradat això de conèixer l'elasticitat de la demanda abans i després, convindria calcular-ho per aquí aprop. Sabem que el consum retail ha caigut un 9,8% en un any i encara no sabem qué han prioritzat els ciutadans davant aquesta impressionant retallada en el consum domèstic.
22 de juliol 2021
15 de juny 2015
The value of vaccination
A PNAS article sets a broader perspective on valuing vaccines. It is of interest in light of current difteria case. My position is clear, no doubt about mandatory vaccination if its cost-effectiveness is proven.
Suggestions from the article:
Three general recommendations flow from our arguments and related synthesis of existing evidence on broad benefits of vaccination. First, many economic evaluation studies of vaccinations should be redone to capture the full benefits generated by the vaccination in question. Second, the evidence to date on the full value of vaccination has been focused on measuring the total social benefits generated. It would also be useful to explore the distribution of vaccination’s benefits among different possible beneficiaries. Third, the primary empirical evidence on broad vaccination benefits will need to be considerably expanded and improved
Framework of vaccination benefits
| Perspective | Benefit categories | Definition | |
| Broad | Narrow | Health care cost savings | Savings of medical expenditures because vaccination prevents illness episodes |
| Care-related productivity gains | Savings of patient’s and caretaker’s productive time because vaccination avoids the need for care and convalescence | ||
| Outcome-related productivity gains | Increased productivity because vaccination improves physical or mental health | ||
| Behavior-related productivity gains | Vaccination improves health and survival, and may thereby change individual behavior, for example by lowering fertility or increasing investment in education | ||
| Community health externalities | Improved outcomes in unvaccinated community members, e.g., through herd effects or reduction in the rate at which resistance to antibiotics develops | ||
| Community economic externalities | Higher vaccination rates can affect macroeconomic performance and social and political stability | ||
| Risk reduction gains | Gains in welfare because uncertainty in future outcomes is reduced | ||
| Health gains | Utilitarian value of reductions in morbidity and mortality above and beyond their instrumental value for productivity and earnings | ||