You'll find inside my article on key issues for population health improvement.
31 de desembre 2019
30 de desembre 2019
How confirmation bias contributes to polarization
Confirmation bias in the utilization of others’ opinion strength
Humans tend to discount information that undermines past choices and judgments. This confirmation bias has significant impact on domains ranging from politics to science and education. Little is known about the mechanisms underlying this fundamental characteristic of belief formation. Here we report a mechanism underlying the confirmation bias. Specifically, we provide evidence for a failure to use the strength of others’ disconfirming opinions to alter confidence in judgments, but adequate use when opinions are confirmatory. This bias is related to reduced neural sensitivity to the strength of others’ opinions in the posterior medial prefrontal cortex when opinions are disconfirming. Our results demonstrate that existing judgments alter the neural representation of information strength, leaving the individual less likely to alter opinions in the face of disagreement.
The notion that the strength of disconfirming opinion is not necessarily proportionate to its impact on belief change is in accord with anecdotal and ‘real-world’ observations in domains ranging from science to politics. The underlying process is remarkably flexible, with the neural circuitry involved switching on a trial-bytrial basis from high sensitivity to relative neglect, contingent on whether the opinion is confirmatory or disconfirming. This process may leave the individual less likely to alter opinions in the face of disagreement.Interesting article from Nature. So what? Is there any exercise to train the neural sensitivity of our posterior medial prefrontal cortex? If so, I would suggest these exercise to some guys.
26 de desembre 2019
Ethical algorithms like hammers?
Main messages:
All decision-making—including that carried out by human beings—is ultimately algorithmic. The difference is that human decision-making is based on logic or behaviors that we struggle to precisely enunciate. If we humans had the ability to describe our own decision-making processes precisely enough, then we could in fact represent them as computer algorithms. So the choice is not whether to avoid using algorithms or not, but whether or not we should use precisely specified algorithms.
Machine learning is a powerful tool that has many extant and potential benefits. Technology companies such as Google and Facebook of course rely on products powered by machine learning for much of their revenue—but as these techniques grow in applicability, their scope and societal benefits grow as well.
The result is that, at least for a while, the critics of the algorithmic approach may often be right. There are many consequential domains where algorithmic tools are still too naive and primitive to be fully trusted with decision-making. This is because to model the forest, we need to start with the trees. This book offers a snapshot of exciting strands of research aimed at developing ethical algorithms, many of which are still in their very earliest days.
23 de desembre 2019
Global pharmaceutical market vs. local regulators
Regulating Medicines in a Globalized World: The Need for Increased Reliance Among Regulators
As defined by the World Health Organization (WHO), recognition occurs when a regulatory authority accepts the regulatory decision of another authority “as its own decision;”— reliance takes place when a regulatory authority takes into account the work products of another authority (e.g., inspection reports, scientific assessment reports, joint assessment reports produced together with another authority) to help inform the receiving authority's own regulatory decision, which, in the end may differ from the made by the initial authority using the same products.Recognition and reliance are the first steps towards an improvement of real coordination between regulatory bodies. If the pharmaceutical market is global, the regulators should cooperate for a coherent global regulation.
22 de desembre 2019
Anchoring and adjusting heuristic
Effect of Teaching Bayesian Methods Using Learning by Concept vs Learning by Example on Medical Students’ Ability to Estimate Probability of a Diagnosis
Why do we need more bayesian reasoning?. Can we improve clinical decision making? The answer in this JAMA article.
Why do we need more bayesian reasoning?. Can we improve clinical decision making? The answer in this JAMA article.
Although bayesian reasoning has been widely promoted in the literature as a diagnostic strategy, there has been scant evidence that teaching bayesian reasoning actually improves diagnostic accuracy. Providing learners with relatively brief instruction on these abstract concepts appeared to significantly improve their diagnostic performance in comparison with simply providing a number of relevant examples or no relevant instruction.
The previously reported discrepancy between human probability estimation and optimal bayesian probability estimation has become traditionally accepted in the psychology and medical literature as cognitive biases, including base-rate neglect, anchoring bias, confirmation bias, and representativeness, all of which suggest suboptimal revision and have been purported to be a primary cause of diagnostic error.13,14 However, on closer scrutiny, much of this evidence was derived from situations that were not representative of the typical diagnostic setting. One highly cited study9 used a screening situation in which the base rate was very low and any positive test result, even one with excellent operating characteristics, would have most likely been a false-positive result. Participants in that study also appeared to exhibit semantic confusion by confusing the posttest probability with the conditional probability that was presented in the problem-solving exercise.
19 de desembre 2019
Medicine as a data science (7)
Artificial Intelligence in Health Care: The Hope, the Hype, the Promise, the Peril
The National Academy of Medicine’s Special Publication: Artificial Intelligence in Health Care: The Hope, The Hype, The Promise, The Peril synthesizes current knowledge to offer a reference document for relevant health care stakeholders such as: AI model developers, clinical implementers, clinicians and patients, regulators, and policy makers, to name a few. It outlines the current and near-term AI solutions; highlights the challenges, limitations, and best practices for AI development, adoption, and maintenance; offers an overview of the legal and regulatory landscape for AI tools designed for health care application; prioritizes the need for equity, inclusion, and a human rights lens for this work; and outlines key considerations for moving forward.A must read
14 de desembre 2019
Pharmaceutical policies
Medicamentos, innovación tecnológica y economía; (2019), nº 160
This issue of Papeles de Economia Española explains the current situation of pharmaceutical policies in Spain. These are the topics:
La industria farmacéutica en la actualidad: un vistazo a sus características
II. LA I+D+I EN LA INDUSTRIA FARMACÉUTICA
La evolución reciente y perspectivas de la innovación
de medicamentos
Ética, medicamentos e innovación
La economía de la I+D en la industria farmacéutica: un resumen
Innovación y competencia en el sector farmacéutico en la época de la medicina de precisión
La innovación y la industria farmacéutica en España
La I+D en el sector farmacéutico español en el período 2003-2015
III. ASPECTOS EMPRESARIALES Y ECONÓMICOS
La evolución de la organización empresarial en la industria farmacéutica
La política de la competencia en la industria farmacéutica
La contribución del sector farmacéutico al crecimiento, a las exportaciones y a la inversión en España
IV. LA PRESTACIÓN FARMACÉUTICA EN LAS COMUNIDADES AUTÓNOMAS
Gestión de la prestación farmacéutica y compras públicas en la Comunidad de Madrid
Procedimiento de selección de medicamentos en atención primaria en Andalucía
La experiencia de gestión de los medicamentos en Cataluña. Objetivos de salud y económicos
V. LA EVALUACIÓN DE LA EFICIENCIA DE LAS INTERVENCIONES Y TECNOLOGÍAS SANITARIAS
La trayectoria metodológica de la evaluación de la eficiencia y su futuro
El valor de las innovaciones médicas
La evaluación de la eficiencia de intervenciones y tecnologías sanitarias en España
VI. LA VISIÓN DEL SECTOR BIOFARMACÉUTICO DESDE LAS EMPRESAS
Industria farmacéutica en España: innovación y compromiso social
El sector de los medicamentos genéricos en España
Medicamentos biosimilares: una oportunidad para el Sistema Nacional de Salud
40 años de autocuidado en España.
Un sector consolidado y emergente
This issue of Papeles de Economia Española explains the current situation of pharmaceutical policies in Spain. These are the topics:
La industria farmacéutica en la actualidad: un vistazo a sus características
II. LA I+D+I EN LA INDUSTRIA FARMACÉUTICA
La evolución reciente y perspectivas de la innovación
de medicamentos
Ética, medicamentos e innovación
La economía de la I+D en la industria farmacéutica: un resumen
Innovación y competencia en el sector farmacéutico en la época de la medicina de precisión
La innovación y la industria farmacéutica en España
La I+D en el sector farmacéutico español en el período 2003-2015
III. ASPECTOS EMPRESARIALES Y ECONÓMICOS
La evolución de la organización empresarial en la industria farmacéutica
La política de la competencia en la industria farmacéutica
La contribución del sector farmacéutico al crecimiento, a las exportaciones y a la inversión en España
IV. LA PRESTACIÓN FARMACÉUTICA EN LAS COMUNIDADES AUTÓNOMAS
Gestión de la prestación farmacéutica y compras públicas en la Comunidad de Madrid
Procedimiento de selección de medicamentos en atención primaria en Andalucía
La experiencia de gestión de los medicamentos en Cataluña. Objetivos de salud y económicos
V. LA EVALUACIÓN DE LA EFICIENCIA DE LAS INTERVENCIONES Y TECNOLOGÍAS SANITARIAS
La trayectoria metodológica de la evaluación de la eficiencia y su futuro
El valor de las innovaciones médicas
La evaluación de la eficiencia de intervenciones y tecnologías sanitarias en España
VI. LA VISIÓN DEL SECTOR BIOFARMACÉUTICO DESDE LAS EMPRESAS
Industria farmacéutica en España: innovación y compromiso social
El sector de los medicamentos genéricos en España
Medicamentos biosimilares: una oportunidad para el Sistema Nacional de Salud
40 años de autocuidado en España.
Un sector consolidado y emergente
12 de desembre 2019
11 de desembre 2019
Laboratory medicine as a data science
Data science, artificial intelligence, and machine learning: Opportunities for laboratory medicine and the value of positive regulation
Jacob Lawrence, This is Harlem, 1943. Gouache and pencil on paper. Hirshhorn Museum and Sculpture Garden, Smithsonian Institution, Gift of Joseph H. Hirshhorn, 1966. Artwork © The Jacob and Gwendolyn Knight Lawrence Foundation, Seattle / Artists Rights Society (ARS), New York; photograph by Cathy Carver
Artificial intelligence (AI) and data science are rapidly developing in healthcare, as is their translation into laboratory medicine.These are the four areas that the authors consider that AI will have impact:
- Processes and care pathways
- Laboratory test ordering and interpretation
- Data mining, early diagnosis, and proactive disease monitoring
- Personalized treatment and clinical trials
Jacob Lawrence, This is Harlem, 1943. Gouache and pencil on paper. Hirshhorn Museum and Sculpture Garden, Smithsonian Institution, Gift of Joseph H. Hirshhorn, 1966. Artwork © The Jacob and Gwendolyn Knight Lawrence Foundation, Seattle / Artists Rights Society (ARS), New York; photograph by Cathy Carver
03 de desembre 2019
The fight between commercialism and professionalism in medicine (3)
The Price We Pay
What Broke American Health Care--and How to Fix It
What Broke American Health Care--and How to Fix It
Health care is perhaps today’s most divisive, territorial political issue. But many of the needed solutions are not partisan; they’re American. We are at a pivotal juncture. Spending on health care threatens every aspect of American society. The time for commonsense reform has arrived. All of us can play a part in driving badly needed reforms, both in the marketplace and in the policy world.
As a society, we should embrace a basic set of patient rights, including a right to obtain a timely quote for a shoppable medical service. Lawmakers should look at the price transparency trails blazed by Florida, New Hampshire, and Maine. The prerequisite of any free market is viewable pricing information—not just inflated charges, but the actual amounts of settled bills. New policies should ensure a level playing field to make the free market functional again, to cut the waste and restore competition to the marketplace.I disagree with the author. Competition it is not the tool for a fairer health care. Wishfull thinking will not drive us to an improvement.
01 de desembre 2019
The fight between commercialism and professionalism in medicine (2)
The Public Creation of the Corporate Health Care System
A second book on the same topic on US healthcare. And the regulatory messages are:
A second book on the same topic on US healthcare. And the regulatory messages are:
Despite the political uproar surrounding the ACA, many citizens, including the legislation's opponents, acknowledged the need for some type of reform. Indeed, ACA antagonists were most effective raising the specter of how federal programming would worsen health care rather than boasting about prevailing arrangements. Poor service distribution, fragmented care, and uneven service quality had long characterized U.S. medicine. But policymakers and voters were primarily concerned about the uninsured and the exorbitant costs that ranked American health care as the world's most expensive. These flaws helped push the ACA over the finish line. And the program has thus far proven resilient, withstanding presidential and congressional contests as well as significant court challenges.Right now it seems that ACA is not enough. Let's wait and see.
The ACA built new rooms atop a defective, jerry-built edifice. The public option would have put the nation firmly on the path toward a nationalized, universal system by creating a government-managed plan and using regulations and mandates to enfeeble and eventually drive out private coverage. Readers can decide for themselves the wisdom of creating a centralized system. Nonetheless, because the ACA failed to secure fundamental, structural reform, it will be unable to rein in costs while also maintaining or improving the quality of care. Indeed, this narrative has illustrated how a fusion of public and private power constructed an institutionally tangled health care system that, even under the banner of comprehensive reform, policymakers were ultimately unable to rescue from the insurance company model.
29 de novembre 2019
The fight between commercialism and professionalism in medicine
Remaking the American Patient
How Madison Avenue and Modern Medicine
Turned Patients into Consumers
I've found this book of interest specially for europeans. Our health systems are currently under pressure. Public budgets are constrained and the private sector is growing. If you want to know what happens next, then this is the book to read. Just to prevent the disaster that comes afterwards, remember that US life expectancy has been declining in the last three years!. Maybe the time to act is now, just to avoid this predictable outcome. Take care.
How Madison Avenue and Modern Medicine
Turned Patients into Consumers
I've found this book of interest specially for europeans. Our health systems are currently under pressure. Public budgets are constrained and the private sector is growing. If you want to know what happens next, then this is the book to read. Just to prevent the disaster that comes afterwards, remember that US life expectancy has been declining in the last three years!. Maybe the time to act is now, just to avoid this predictable outcome. Take care.
28 de novembre 2019
Digital health transformation
Health in the 21st Century
Putting Data to Work for Stronger Health Systems
A new report by OECD highlights the potential digital health environment. We are still far from what they say. However, while reading it you'll be aware of its relevance. Chapter 5 is a must read:
Putting Data to Work for Stronger Health Systems
A new report by OECD highlights the potential digital health environment. We are still far from what they say. However, while reading it you'll be aware of its relevance. Chapter 5 is a must read:
Big data, and big data analytics, can be used at all three levels of health promotion and disease prevention – research, surveillance, and intervention – by:
-Allowing a more precise identification of at-risk populations, through a more comprehensive understanding of human health and disease, including the interaction between genetic, lifestyle, and environmental determinants of health;
-Enabling better surveillance of both communicable and non-communicable diseases; and
- Facilitating better targeted strategies and interventions to improve health promotion and
disease prevention.
21 de novembre 2019
Against the riggers
El enemigo conoce el sistema
Manipulación de ideas, personas e influencias después de la economía de la atención
Manipulación de ideas, personas e influencias después de la economía de la atención
Uno de los errores recurrentes de la izquierda es pensar que el populismo es la estrategia de los imbéciles, cuando la historia demuestra que no puede ser tan imbécil cuando consigue un éxito arrollador. Ya en Los orígenes del totalitarismo, Hannah Arendt explica que este tipo de estrategia está diseñada deliberadamente para desprender a la sociedad educada de sus recursos intelectuales y espirituales, convirtiendo a la población en cínicos o en niños, dependiendo del ego y el aguante de cada uno. Una doctrina del shock que precede a la escuela de Chicago y que ha sido característica de todos los totalitarismos contemporáneos, del nazismo alemán al estalinismo ruso, pasando por el fascismo italiano.En un mundo eternamente cambiante e incomprensible, las masas han llegado hasta el punto de que podrían, al mismo tiempo, creer todo o nada, pensar que todo era posible y que nada era verdad... Los líderes de masas totalitarios basaban su propaganda en la correcta premisa psicológica de que, en esas condiciones, uno podía hacer que la gente creyera la declaración más fantasiosa un día, y saber que si al día siguiente les dieran la prueba irrefutable de su falsedad, encontrarían refugio en el cinismo. En lugar de abandonar a los líderes que les habían mentido, clamarían que supieron en todo momento que la declaración era mentira y admirarían a los líderes por su agudeza táctica superior.
08 de novembre 2019
How much do countries spend on health?
Health at a Glance 2019: OECD Indicators
The european country that spends the most is Switzerland 12,2% over GDP. In Catalonia this figure was 7,6% in 2016 (less than Greece). Per capita income in 2016 was 35% more in Switzerland than in Catalonia, while health expenditure was 60% more in Switzerland. Where have the catalan taxes gone?. You know it and I know it. And everybody is aware that there is only one solution to have the appropriate public health expenditure. We have to say good bye as soon as possible.
The european country that spends the most is Switzerland 12,2% over GDP. In Catalonia this figure was 7,6% in 2016 (less than Greece). Per capita income in 2016 was 35% more in Switzerland than in Catalonia, while health expenditure was 60% more in Switzerland. Where have the catalan taxes gone?. You know it and I know it. And everybody is aware that there is only one solution to have the appropriate public health expenditure. We have to say good bye as soon as possible.
07 de novembre 2019
How to identify lab tests of low effectiveness?
Prevalence and Predictability of Low-Yield Inpatient Laboratory Diagnostic Tests
A new approach to understand the size of useless lab tests is to apply: "regularized logistic regression, regress and round, naive Bayes, neural network multilayer perceptrons, decision tree, random forest, AdaBoost, and XGBoost". This means that machine learning has its own space in laboratory medicine. In the article, they show high level of prediction for useless tests.
A new approach to understand the size of useless lab tests is to apply: "regularized logistic regression, regress and round, naive Bayes, neural network multilayer perceptrons, decision tree, random forest, AdaBoost, and XGBoost". This means that machine learning has its own space in laboratory medicine. In the article, they show high level of prediction for useless tests.
The best performing machine learning models predicted normal results with an AUROC of 0.90 or greater for 12 stand-alone laboratory tests (eg, sodium AUROC, 0.92 [95%CI, 0.91-0.93]; sensitivity, 98%; specificity, 35%; PPV, 66%; NPV, 93%; lactate dehydrogenase AUROC, 0.93 [95%CI, 0.93-0.94]; sensitivity, 96%; specificity, 65%; PPV, 71%; NPV, 95%; and troponin I AUROC, 0.92 [95%CI, 0.91- 0.93]; sensitivity, 88%; specificity, 79%; PPV, 67%; NPV, 93%) and 10 common laboratory test components (eg, hemoglobin AUROC, 0.94 [95%CI, 0.92-0.95]; sensitivity, 99%; specificity, 17%; PPV, 90%; NPV, 81%; creatinine AUROC, 0.96 [95%CI, 0.96-0.97]; sensitivity, 93%; specificity, 83%; PPV, 79%; NPV, 94%; and urea nitrogen AUROC, 0.95 [95%CI, 0.94, 0.96]; sensitivity, 87%; specificity, 89%; PPV, 77%; NPV 94%).This approach goes further than this book:
03 de novembre 2019
It's always about quality
La qualité des services de santé. Un impératif mondial en vue de la couverture santé universelle
Improving healthcare quality in Europe. Characteristics, effectiveness and implementation of different strategies
Improving healthcare quality in Europe. Characteristics, effectiveness and implementation of different strategies
The essential element of access to healthcare overshadows the understanding that better health can only be achieved if accessed services are also of high quality. The Sustainable Development Goals spell this out quite clearly: “Achieve universal health coverage, including financial risk protection, access to quality essential health-care services and access to safe, effective, quality and affordable essential medicines and vaccines for all” (Goal 3, Target 8). Indeed, ensuring that healthcare services are of good quality is an imperative for policy-makers at all levels and an important contributor to health system performance.
02 de novembre 2019
Eurohealth
Everything you always wanted to know about European Union health policies but were afraid to ask
I have to say that I am not afraid to ask about health policies in EU because EU is basically a market. Therefore nothing to ask. Social policy is out of the real scope of EU.However, as a regulator of the market for health has clear examples of disfunctioning. For example, implantable medical devices regulation currently applied was enacted in 1990. New regulation will be applied next year, after 30 years of regulatory vacation. Nothing to add. Taxes haven't been on vacation. Shame on Europe. By the way, you'll not find minor details like this one in the book.
I have to say that I am not afraid to ask about health policies in EU because EU is basically a market. Therefore nothing to ask. Social policy is out of the real scope of EU.However, as a regulator of the market for health has clear examples of disfunctioning. For example, implantable medical devices regulation currently applied was enacted in 1990. New regulation will be applied next year, after 30 years of regulatory vacation. Nothing to add. Taxes haven't been on vacation. Shame on Europe. By the way, you'll not find minor details like this one in the book.
01 de novembre 2019
The impact of an ageing population (2)
Working Better With Age
WORKING AT OLDER AGES
Why it’s important, how it affects health, and the policy options to support health capacity for work
The message of OECD report:
WORKING AT OLDER AGES
Why it’s important, how it affects health, and the policy options to support health capacity for work
The message of OECD report:
The number of older inactive people who will need to be supported by each worker could rise by around 40% between 2018 and 2050 on average in the OECD area. This would put a brake on rising living standards as well as enormous pressure on younger generations who will be financing social protection systems. Improving employment prospects of older workers will be crucial. At the same time, taking a life-course approach will be necessary to avoid accumulation of individual disadvantages over work careers that discourage or prevent work at an older age; What can countries do to help? How can they give older people better work incentives and opportunities? This report provides a synthesis of the main challenges and policy recommendations together with a set of international best practices to foster employability, labour demand and incentives to work at an older age.And the WHO report message:
Dominant policy approaches such as increasing the statutory retirement age are often overshadowed by a lack of attention to two critical questions: firstly, are older workers in sufficiently good health to work longer? And secondly, does increasing the statutory retirement age have consequences, negative or positive, for the health of older workers?
29 d’octubre 2019
The impact of an ageing population
Sustainable health financing with an ageing population: implications of different revenue raising mechanisms and policy options
Sustainable health financing with an ageing population: Will population ageing lead to uncontrolled health expenditure growth?
Three documents from WHO Europe are available regarding financing health for an ageing population. You can skip the third, it is about predictions for 2060. This is useless as I've said many times.
However, I agree with this comment:
Sustainable health financing with an ageing population: Will population ageing lead to uncontrolled health expenditure growth?
Three documents from WHO Europe are available regarding financing health for an ageing population. You can skip the third, it is about predictions for 2060. This is useless as I've said many times.
However, I agree with this comment:
These analyses find that population ageing is not, and will not become, a major driver of growth in health expenditures. Moreover, they suggest that in countries where age demographics are changing but the size of the older population is not yet large, the costs of improving coverage and access to services for older people is likely to be manageable and now is a good time to begin investing in the health system while the population is relatively young.
However, while population ageing will not become a main driver of health expenditure growth, policy choices related to how health services are delivered, the prices paid (or negotiated) for services, medicines and technologies, and volumes of care will ultimately determine health spending by age trends.
25 d’octubre 2019
The end of social health insurance
Social Health Insurance in Europe: Basic Concepts and New Principles
During the first decade of this century, health reforms have advocated for universal health coverage in those countries with social health insurance based on contributions. This is a strong trend that needs to be evaluated. A recent article describes in detail these changes and says:
During the first decade of this century, health reforms have advocated for universal health coverage in those countries with social health insurance based on contributions. This is a strong trend that needs to be evaluated. A recent article describes in detail these changes and says:
Contrary to some expectations, SHI in Europe has further expanded toward universal coverage, with access to health care considered a right based on either direct or indirect financial contributions. Indeed, Germany is now the only example in Europe where groups of the population can opt out from the main insurance system. And, since 2009, the overall population is required to be covered by either social or private insurance.
24 d’octubre 2019
The world is fat
The Heavy Burden of Obesity – The Economics of Prevention
Almost a decade after the publication of the first OECD report on obesity, a new one has been released. This are the facts:
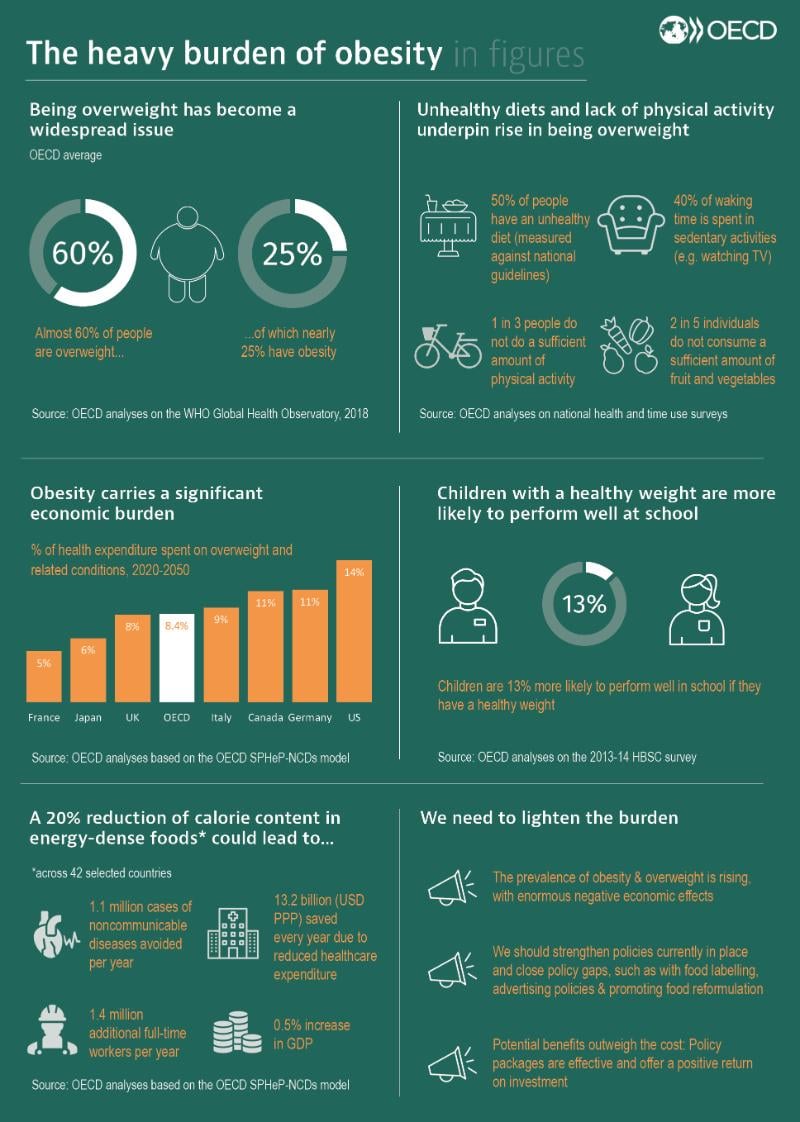
Almost a decade after the publication of the first OECD report on obesity, a new one has been released. This are the facts:
More than half the population is now overweight in 34 out of 36 OECD countries and almost one in four people is obese. Average rates of adult obesity in OECD countries have increased from 21% in 2010 to 24% in 2016, so an additional 50 million people are now obese. Despite a drive in the last decade to deal with increased obesity, more needs to be done amid sedentary lifestyles and an almost 20% increase in calorie supply – i.e. calories available for consumption – in the OECD over the past 50 years.So what?
The OECD identifies four categories of policies to tackle the problem and gauges the effect of three promising “policy packages” to help countries achieve greater impact and coherence in tackling the obesity epidemic. Food and menu labelling, regulation of advertising of unhealthy foods to children and the promotion of exercise, including by doctors and schools, are among the measures analysed.Most of the strategies requires a confrontation with the food industry, and governments usually try to avoid it. We'll see what happens.

16 d’octubre 2019
Gen-ethics (2)
Special Issue: The Ethics Of Human Genome Editing
The CRISPR journal has released a special issue on ethics. You'll find an article with the title "Heritable Genome Editing and the Downsides of a Global Moratorium". This is exactly the opposite argument that Françoise Baylis provides in her book. I think that it is unacceptable a recommendation that nations should "regulate HGE for safety and efficacy only and without distinguishing between therapeutic and enhancing modifications". We can't leave such decisions to scientists and practitioners. I'm really concerned about it.
The CRISPR journal has released a special issue on ethics. You'll find an article with the title "Heritable Genome Editing and the Downsides of a Global Moratorium". This is exactly the opposite argument that Françoise Baylis provides in her book. I think that it is unacceptable a recommendation that nations should "regulate HGE for safety and efficacy only and without distinguishing between therapeutic and enhancing modifications". We can't leave such decisions to scientists and practitioners. I'm really concerned about it.
10 d’octubre 2019
Gen-ethics
Altered Inheritance
CRISPR and the Ethics of Human Genome Editing
Our future belongs to all of us. Or maybe not? Maybe somebody could decide for us without noticing it?. The "decisions about the use of genetic technologies in humans are too important to be left to scientists", society has to achieve a broad consensus. Françoise Baylis in her new book sheds light on this issue. She explained his position in an article last spring and now she has published a remarkable book on ethics and genome editing. Her calls for an open and comprehensive international process to reach political, scientific, and social/ethical consensus on regulation of human genome editing have been unattended up to now. Her ultimate goal:
CRISPR and the Ethics of Human Genome Editing
Our future belongs to all of us. Or maybe not? Maybe somebody could decide for us without noticing it?. The "decisions about the use of genetic technologies in humans are too important to be left to scientists", society has to achieve a broad consensus. Françoise Baylis in her new book sheds light on this issue. She explained his position in an article last spring and now she has published a remarkable book on ethics and genome editing. Her calls for an open and comprehensive international process to reach political, scientific, and social/ethical consensus on regulation of human genome editing have been unattended up to now. Her ultimate goal:
I want to live in a world that promotes equity and justice and celebrates difference, a world where everyone matters. I want to live in a world where we embrace neighborliness, reciprocity, social solidarity, and community in pursuit of human flourishing and the common good. I want to live in a world where we value collegial as opposed to competitive relations. I don’t want to live in a world where a select, privileged few are able to inscribe their privilege in their DNA and thereby exacerbate unfair class divisions and other social injustices. For these reasons, I want for all of us to reflect on whether heritable human genome editing is a boon or a threat.I agree. An essential reading highly recommended.
03 d’octubre 2019
Social differences in health and health systems
Health for Everyone?
Social Inequalities in Health and Health Systems
I still don't know why do we talk about inequalities, I've always thought that we should care about differences. The word inequality drives your mind towards equality, and we all know that this will not happen. Therefore, there are differences that are unfair and avoidable, and these are the ones we have to be concerned.
And when we talk bout social determinants, maybe we should focus on commercial determinants and it would help. Why commercial? Because these factors are more actionable compared to others.
You will not find all these reflections in the new report by OECD. Anywasy it is worth reading to confirm it, though the perspective is the standard one (Marmot) and not new.
What you really have to read is the notice at the begining of each chapter that says:
PS. What I said in the blog on Cyprus 8 years ago:
Social Inequalities in Health and Health Systems
I still don't know why do we talk about inequalities, I've always thought that we should care about differences. The word inequality drives your mind towards equality, and we all know that this will not happen. Therefore, there are differences that are unfair and avoidable, and these are the ones we have to be concerned.
And when we talk bout social determinants, maybe we should focus on commercial determinants and it would help. Why commercial? Because these factors are more actionable compared to others.
You will not find all these reflections in the new report by OECD. Anywasy it is worth reading to confirm it, though the perspective is the standard one (Marmot) and not new.
What you really have to read is the notice at the begining of each chapter that says:
Note by Turkey:Shame on Turkey. This notice is an example of the decision that needs to take the OECD urgently: to exclude Turkey from his organization. It is really unacceptable what Turkey has done and it is doing in Cyprus. Europe and OECD are avoiding the conflict saying "The information in this document relates to the area under the effective control of the Government of the Republic of Cyprus". The conflict should be solved as soon as possible with the withdrawal of Turkey from Cyprus. That's all.
The information in this document with reference to “Cyprus” relates to the southern part of the Island. There is no single authority representing both Turkish and Greek Cypriot people on the Island. Turkey recognises the Turkish Republic of Northern Cyprus (TRNC). Until a lasting and equitable solution is found within the context of the United
Nations, Turkey shall preserve its position concerning the “Cyprus issue”.
Note by all the European Union Member States of the OECD and the European Union:
The Republic of Cyprus is recognised by all members of the United Nations with the exception of Turkey. The information in this document relates to the area under the effective control of the Government of the Republic of Cyprus.
PS. What I said in the blog on Cyprus 8 years ago:
PS. Carta de lluny. Tot d'una passejant pel carrer Ledra vaig topar amb una frontera. Em trobava a una capital europea, dividida, envaïda. L'illa de Xipre va quedar escapçada el 1974. Aquella invasió va provocar 200.000 desplaçats que van perdre-ho tot fins el dia d'avui. El genocidi cultural i el saqueig posterior encara dura. He tingut ocasió de visitar dues exposicions que mostren l'espoli que s'està produint a la regió de Morphou (pot visitar-se al Banc de Xipre) i el rescat d'algun botí d'antiquari de l'any passat a Alemanya (Makarios Foundation). Vaig quedar tocat en veure-ho. Tresors artístics destruits per tal que la cultura d'altres desaparegui definitivament. Molt fort.
La situació política és delicada després de l'explosió de l'arsenal de Limassol a mitjans de juliol. Vam assistir a concerts on l'electricitat la subministràven amb generadors, i a Limassol moltes botigues no tenien llum. Tenen una bombolla urbanística com una catedral i està a punt d'esclatar.
L'escapada cap al Nord va tenir tres destins: Salamina, Famagusta i Kyrenia. Arribar a Salamina suposava fer un visat i assegurança del cotxe però el difícil era arribar-hi perquè no hi havia cap cartell. Salamina és un complex interessant però descuidat i menystingut. Famagusta té una mescla que em va sobtar visualment, catedrals gòtiques escapçades amb minarets. Havia de ser extraordinària però s'han encarregat deliberadament de destruir-la, s'observa clarament quan passeges. Kyrenia va ser un descans, lloc acollidor. Al port amb una calor sofocant vam passar una bona estona. Vam oblidar per pocs moments el país envaït on ens trobàvem.
Crec que els governs que faciliten, impulsen o s'inhibeixen davant del genocidi cultural haurien de ser exclosos del circuit, pena d'infàmia, cosa que per ara no fa ningú.
Hem tingut ocasió de visitar Pafos, els Troodos i les esglésies patrimoni de la humanitat, Kourion, i molts altres llocs. El menjar i en especial la qualitat del peix és envejable. Un bon record i una experiència més per a compartir.
30 de setembre 2019
Digitization
Digital Economics
If you want to get a description of what digital economics represents, this article in JEL is the one you have to read.
If you want to get a description of what digital economics represents, this article in JEL is the one you have to read.
Digital economics explores how standard economic models change as certain costs fall substantially and perhaps approach zero. We emphasize how this shift in costs can be divided into five types:Its impact in healthcare is starting right now. Platforms that allow communication between physicians and patients leverage such digital environments. However, all these platforms have admitted that personal contact can't be avoided. Right now, digital represents a small part. Everything will not be digital, at least in healthcare.
(i) Lower search costs
(ii) Lower replication costs
(iii) Lower transportation costs
(iv) Lower tracking costs
(v) Lower verification costs
Boudin at Mapfre Foundation in Barcelona
26 de setembre 2019
Improving population health (2)
References of my speech
Carreras, Marc, et al. "Morbilidad y estado de salud autopercibido, dos aproximaciones diferentes al estado de salud." Gaceta Sanitaria (2019).
Postman, Neil. Amusing ourselves to death: Public discourse in the age of show business. Penguin, 2006.
Lakoff, George. The political mind: why you can't understand 21st-century politics with an 18th-century brain. Penguin, 2008.
Barer, Morris L., et al., eds. An Undisciplined Economist: Robert G. Evans on Health Economics, Health Care Policy, and Population Health. McGill-Queen's Press-MQUP, 2016.
Pere Ibern, Jordi Calsina. Més enllà de la separació de funcions: organitzacions sanitàries integrades. Fulls econòmics del sistema sanitari, Nº 35, 2001, págs. 17-20
Harris, Jeffrey E. "The internal organization of hospitals: some economic implications." The Bell Journal of Economics (1977): 467-482.
Freidson, Eliot. Professionalism, the third logic: On the practice of knowledge. University of Chicago press, 2001.
Topol, Eric. The patient will see you now: the future of medicine is in your hands. Basic Books, 2015.
Kindig, David, and Greg Stoddart. "What is population health?." American journal of public health 93.3 (2003): 380-383.
Mateu i Serra, Antoni. "Salud en Todas las Políticas e intersectorialidad en la promoción de la salud: el Plan Interdepartamental de Salud Pública (PINSAP) de Cataluña." Medicina Clínica 145.Extr. 1 (2015): 34-37.
Verschuuren, Marieke, and Hans Van Oers, eds. Population Health Monitoring: Climbing the Information Pyramid. Springer, 2018.
Hansen, Pelle Guldborg. "BASIC: Behavioural Insights Toolkit and Ethical Guidelines for Policy Makers." (2018).
Kahneman, Daniel. Thinking, fast and slow. Macmillan, 2011.
Courtwright, David T. The Age of Addiction: How Bad Habits Became Big Business. Harvard University Press, 2019.
Kindig, David A. Purchasing population health: paying for results. University of Michigan Press, 1997.
Baciu, Alina, and Joe Alper, eds. Financing Population Health Improvement: Workshop Summary. National Academies Press, 2015.
Carreras, Marc, et al. "Morbilidad y estado de salud autopercibido, dos aproximaciones diferentes al estado de salud." Gaceta Sanitaria (2019).
Postman, Neil. Amusing ourselves to death: Public discourse in the age of show business. Penguin, 2006.
Lakoff, George. The political mind: why you can't understand 21st-century politics with an 18th-century brain. Penguin, 2008.
Barer, Morris L., et al., eds. An Undisciplined Economist: Robert G. Evans on Health Economics, Health Care Policy, and Population Health. McGill-Queen's Press-MQUP, 2016.
Pere Ibern, Jordi Calsina. Més enllà de la separació de funcions: organitzacions sanitàries integrades. Fulls econòmics del sistema sanitari, Nº 35, 2001, págs. 17-20
Harris, Jeffrey E. "The internal organization of hospitals: some economic implications." The Bell Journal of Economics (1977): 467-482.
Freidson, Eliot. Professionalism, the third logic: On the practice of knowledge. University of Chicago press, 2001.
Topol, Eric. The patient will see you now: the future of medicine is in your hands. Basic Books, 2015.
Kindig, David, and Greg Stoddart. "What is population health?." American journal of public health 93.3 (2003): 380-383.
Mateu i Serra, Antoni. "Salud en Todas las Políticas e intersectorialidad en la promoción de la salud: el Plan Interdepartamental de Salud Pública (PINSAP) de Cataluña." Medicina Clínica 145.Extr. 1 (2015): 34-37.
Verschuuren, Marieke, and Hans Van Oers, eds. Population Health Monitoring: Climbing the Information Pyramid. Springer, 2018.
Hansen, Pelle Guldborg. "BASIC: Behavioural Insights Toolkit and Ethical Guidelines for Policy Makers." (2018).
Kahneman, Daniel. Thinking, fast and slow. Macmillan, 2011.
Courtwright, David T. The Age of Addiction: How Bad Habits Became Big Business. Harvard University Press, 2019.
Kindig, David A. Purchasing population health: paying for results. University of Michigan Press, 1997.
Baciu, Alina, and Joe Alper, eds. Financing Population Health Improvement: Workshop Summary. National Academies Press, 2015.
23 de setembre 2019
Improving population health
My speech at Reial Acadèmia de Medicina de les Illes Balears
Aspectos clave para la mejora de la salud poblacional, una agenda para la acción
Quisiera agradecer en primer lugar la oportunidad de ofrecerles hoy unas reflexiones sobre las cuestiones fundamentales para la mejora de la salud poblacional y algunas pistas para llevarlas a la práctica. La salud y el bienestar de una población toma como punto de referencia inicial la esperanza de vida. Tenemos buenas noticias en este sentido, en Balears en los últimos 15 años, la esperanza de vida ha aumentado una media de 3 años. Para los hombres se sitúa en 80,9 años y para las mujeres en 85,8. Sin embargo, el dato clave es la esperanza de vida en buena salud. Que para los hombres está en 69,2 y en las mujeres en 68,2 (con datos referidos a 2016). Es decir que los hombres pasan el 85% y las mujeres un 79% de la vida en buena salud, es decir en sin limitaciones funcionales o discapacidad. Diez años antes, en 2006, los hombres vivían en buena salud 61 años, un 78% de su vida y las mujeres 60, un 72% de su vida. En 10 años se ha aumentado la vida en buena salud en 7 puntos. Este es un hito dificil de replicar en el futuro porque podemos esperar una tasa marginal de crecimiento más limitada.
Se confirma pues que en la pasada década el mayor aumento se ha producido en los años de vida en buena salud, casi 3 veces más que el aumento de la esperanza de vida al nacer. Este dato debemos recordarlo como fundamental. Interesa la longevidad pero todavía más la calidad de vida en términos marginales. Hasta aquí, he hablado de la media, sin embargo desconocemos como se distribuye este nivel de salud con precisión.
Además convendrá recordar que este cambio ha coincidido en buena parte con la gran recesión económica que hemos vivido. Una situación económica excepcional que en resumen y para referirnos a los mismos años anteriores (2006-2016) la renta per cápita aumentó tan sólo un 3% en Balears. Y además, el nivel de desigualdad económica de las familias se ha agravado como no habíamos conocido nunca en tan poco tiempo. La OCDE ha mostrado que si medimos la desigualdad mediante los cambios en renta disponible, el Estado Español encabeza el conjunto de los 30 países, con un fuerte diferencial. Esta ha sido una situación desconocida para toda nuestra generación que habíamos vivido en un proceso continuado de crecimiento económico. El resultado es que a fecha de hoy el peso de la clase media se ha reducido, mientras que el de las clases bajas ha crecido en la misma proporción. Aun así, la clase media todavía representa el 58% de la población de Balears en 2017.
Es cierto que en unos momentos de cambio económico y social acelerado, el sector salud se vea afectado de forma profunda dada su relevancia en los ciudadanos. Y también es bueno recordar que todos aquellos que anunciaban que el gasto sanitario crecería de forma natural porque la tecnología y el envejecimiento era imparables, es bueno recordarles precisamente que no ha sido así. Hemos tenido envejecimiento en esta década pasada, ha habido innovación tecnológica y hemos conseguido mejorar la esperanza de vida en buena salud con una restricción presupuestaria absoluta, desconocida por muchos de nosotros. Todos los que pregonaban que el gasto era inevitable ahora deberían analizar detenidamente lo que ha sucedido realmente, pero desafortunadamente las dinámicas coyunturales evitan tal reflexión. El gran economista de la salud, Bob Evans, en los años 90 ya había afirmado que la inevitabilidad del gasto sanitario era una falacia, la gran recesión ha tenido la ocasión de confirmarlo.
Conviene reflejar además que la satisfacción ciudadana con el sistema sanitario público se ha mantenido durante estos años. Este es un hecho más que notable, que hay que destacar en un contexto adverso.
Nos encontramos ante un sistema de salud que alcanza unos resultados buenos, más que notables con los recursos que dedicamos. El gran periodista Antoni Bassas decía: Cualquiera que haya ido por el mundo, y no sólo para países más pobres que Cataluña, sino también para países de la Unión Europea, reconocerá que con recortes o sin, en materia de sanidad no sabemos lo que tenemos. Cientos de millones de personas en todo el mundo darían lo que no tienen para poder llevar en el bolsillo una tarjeta que los cubre como nos cubre a nosotros nuestra tarjeta sanitaria.
Estoy convencido de que la mayoría de los que estamos aquí compartimos sus palabras. Entonces, podemos preguntarnos qué justifica que la sanidad sea motivo de tanta controversia, que se nieguen los hechos y que se haga un uso partidista de los argumentos políticos. Esto tiene que ver con varios factores, pero dejadme que en destaque dos: "los medios" y "los marcos de referencia". Vivimos en un tiempo donde la política está secuestrada por lo que Neil Postman tildaba de "show business". Este gran sociólogo escribió en 1985 un libro premonitorio muy recomendable, titulado: "Divertirse hasta morir, el discurso público en la era del show business".
Decía al final del libro: Lo que yo sugiero es lo que decía también Aldous Huxley, estamos en una carrera entre la educación y el desastre, y necesitamos entender la política y la epistemología de los medios de comunicación. Lo que aquejaba a la gente del El mundo feliz no era que estuvieran riendo en lugar de pensar, sino que no sabían de qué estaban riendo y porqué habían dejado de pensar ". Este es un texto escrito antes de la existencia de internet y las redes sociales. No añadiré nada más. La banalización de la cultura y de la política se ha impuesto y nos conviene volver al espíritu crítico fundamentado y al debate respetuoso, aquel que nos hace progresar como sociedad y como personas.
La segunda cuestión que quería destacar proviene de la ciencia cognitiva, en concreto del profesor de Berkeley, George Lakoff y que ahora es conocido por su libro "No pienses en un elefante". Dice: Los marcos de referencia son estructuras mentales que conforman nuestro modo de ver el mundo, conforman los objetivos que nos proponemos, los planes que hacemos, nuestra forma de actuar y lo que cuenta como resultado bueno o malo de nuestras acciones. En política, los marcos conforman nuestras políticas sociales y las instituciones. Cambiar nuestros marcos es cambiar todo esto. Los marcos de referencia no pueden verse ni sentirse, forman parte del inconsciente cognitivo, estructuras de nuestro cerebro a las que no podemos acceder conscientemente, pero que conocemos por sus consecuencias: nuestra forma de pensar y lo que se entiende por sentido común.
Sigo los trabajos de George Lakoff desde hace años y estoy convencido de que nos puede proporcionar la clave para comprender qué está sucediendo en la política y la gestión sanitaria: nos encontramos ante un nuevo marco de referencia que lucha con lo que hemos convivido durante muchos años y que nos mantenía en lo que los psicólogos llaman "zona de confort".
***
Hace tiempo un periodista me preguntaba, me decía Pere, qué crees que necesita el sistema de salud catalán: más financiación o mejor organización?. Yo le dije que la respuesta no era posible lo uno sin lo otro, necesitábamos ambas cosas. Él sin duda quería un titular, y eso ya no cabía. Hay que estar atento a los falsos dilemas y no dejarnos embaucar.
Necesitamos más financiación si somos capaces de demostrar cuál es el valor marginal obtenido de cada euro adicional gastado. De lo contrario me resisto a señalar cuál es el nivel de financiación necesario y cuidadoso. Sin embargo, ya sabemos que el debate sanitario pivota demasiado sobre cuánto dinero nos gastamos y demasiado poco en que obtenemos a cambio. Demasiado en la financiación y poco en la organización.
Por otro lado, hace más de tres décadas que una Constitución dijo que los ciudadanos éramos iguales ante la ley, pero en cambio podemos observar que cuando hay concierto económico, unos ciudadanos pueden gastar en sanidad pública un 40% más que nosotros en el marco de un mismo Estado de Derecho. Lo que tenemos desde entonces es un estado del revés, una chapuza. En un estado del revés nadie puede pensar seriamente en criterios objetivos, ni fijar prioridades, primero hay que ponerlo del derecho. Esto no ha sido posible desde hace muchas, muchas décadas.
Por lo tanto necesitamos mejor financiación en un marco donde podamos priorizar los recursos para alcanzar un valor mayor en salud, y esto sólo será posible en un marco político de referencia nuevo.
***
Pero al mismo tiempo necesitamos mejor organización. Y permítanme una autocita, esta vez del 2001. En un artículo en la revista Fulls Económics del Sistema Sanitari, junto con el amigo Jordi Calsina, escribimos un artículo titulado: "Más allá de la separación de funciones: las organizaciones sanitarias integradas ". Hace dieciocho años que algunos ya nos habíamos dado cuenta de que había que cambiar de marco de referencia en el aspecto organizativo. Han pasado años y nos hemos mantenido en una "zona de confort". Había que ir más allá de la separación de funciones para que algunos vemos que era un concepto difuso, complicado de llevar a cabo en la práctica en un entorno donde la transferencia de riesgo sólo se sostiene sobre el papel. Y proponíamos las organizaciones sanitarias integradas en la medida que cambiaba la lógica de la compra de servicios por el compromiso con la salud de la comunidad por parte de todos los proveedores.
He estado siguiendo y todavía sigo de cerca el esfuerzo hecho desde Palamós por los Servicios Sanitarios Integrados del Baix Empordà, enfocado hacia una visión de servicio integradora. No es por casualidad que un residente distinguido como el novelista Tom Sharpe escribía con claridad en The Guardian sobre la calidad de servicio que recibió y consideraba que nunca el NHS lo hubiera tratado igual. Más allá de esta anécdota, si me preguntaran por un modelo organizativo apropiado sería este, evidentemente como siempre mejorable.
Tenemos un sistema público de salud con unas características organizativas singulares destacables, citaré dos solamente. La primera es la planificación de recursos, el mapa sanitario, la condición previa a cualquier desbarajuste inversor y al exceso de capacidad instalada que suele suceder en entornos privados. La segunda es la inexistencia del pago por acto médico, motivo de fragmentación, sobrediagnóstico y exceso de tratamiento a muchos sistemas de salud. Aquellos que aún lo aplican luchan por una alternativa.
Ahora bien, el ejercicio responsable de la gobernanza de las organizaciones ha sido posiblemente la pieza más olvidada del engranaje del sistema público de salud. Algunas de las controversias del momento nos las hubiéramos podido ahorrar si hubiéramos dedicado más esfuerzos a estructurar la función de gobierno. Como siempre generalizar tiene riesgos, y por lo tanto ha habido casos ejemplares de gobernanza pero que en mi opinión han sido aislados.
***
Y llegados hasta aquí, hay que recordar las singularidades del entorno de la gestión sanitaria. En Jeffrey Harris, economista y médico, profesor del MIT y internista al Hospital General de Massachussets escribió en 1977 un extraordinario artículo titulado: "La organización interna de los hospitales, algunas implicaciones económicas". Tengo que confesar que fue uno de los primeros artículos de economía de la salud que leí y que me impactó. Pero no sólo a mí, es uno de los artículos más referenciados que hay a fecha de hoy. Esencialmente en Jeffrey Harris dijo en otras palabras, algunas cosas que sabemos los que hemos sido gerentes de hospital. Él sugería que el hospital en realidad son dos empresas: la administrativa y la médica. En esta organización dual hay un conjunto de reglas implícitas de asignación de recursos. La controversia se produce cuando la demanda médica supera la capacidad ofrecida por la administrativa. Nos enfocamos demasiado a analizar la parte administrativa y no tanto a la médica. Y terminaba señalando que hay una nueva organización interna de los hospitales.
Ahora si tuviera que reescribir el artículo seguro que iría más allá de los hospitales y pensaría en organizaciones sanitarias integradas. Considero que Harris acertó en el diagnóstico pero se quedó corto en la terapia, se quedó a medias. Hay que repensar muy seriamente la posición de los médicos dentro de la organización sanitaria. Estoy convencido de que el encaje actual chirría, y las propuestas para avanzar son limitadas. Después de observar modelos alternativos, he llegado al convencimiento de que la relación laboral de la profesión médica en un convenio colectivo difícilmente encaja con la realidad de la tarea, el talento y los resultados que se esperan. Si dentro de la relación laboral tengo dudas, imaginen los que tendré si hay una atribución funcionarial vitalicia, en propiedad, como lo llaman. A fecha de hoy todavía tengo pendiente de encontrar a alguien que me justifique que un médico debe ser funcionario con un argumento convincente.
Para enfocar una visión alternativa, es necesario comprender la profesión médica en el marco organizativo del sistema de salud con las coordenadas inherentes del profesionalismo.
Hay que ser precisos en lo que estamos hablando. Entiendo el profesionalismo más allá de la autonomía estricta y sesgada que algunos defienden. Para profesionalismo quiero decir: (1) altruismo, en caso de conflicto de interés entre intereses profesionales y los de los pacientes, hay que decantarse en favor de los pacientes, (2) un compromiso en la mejora, los profesionales deben actualizarse en el nuevo conocimiento y su incorporación a la práctica (3) revisión entre colegas, los médicos deben ser capaces de supervisar el trabajo de los colegas, para proteger a los pacientes y (4) los médicos deben incorporar el criterio de eficiencia social en las decisiones clínicas.
Si pensamos en una integración asistencial exitosa, necesitamos que la coordinación y motivación en el ámbito clínico sea máxima. En la actualidad, muchos de los avances obtenidos han tenido relación con la capacidad de liderazgo y la cultura organizativa, aunque los incentivos explícitos han sido escasos. La prueba definitiva de que puede llegar más allá en la integración es cuando los profesionales se implican porque más allá de los atributos del profesionalismo, sienten que su esfuerzo se ve compensado y respetado. Muy a menudo, la segunda cuestión toma más importancia que la primera, quiero decir que el respeto ocupa una posición superior a la compensación material. Valorar el trabajo bien hecho, reconocerlo, es fundamental en el entorno profesional. En esto, la sociedad profesional es capaz de hacerlo mejor que tal como lo hace la parte administrativa de la organización hoy en día.
***
Estamos asistiendo a un cambio profundo en la "función de producción de salud". En el libro del cardiólogo Eric Topol titulado "El paciente te atenderá", quiere señalar las nuevas capacidades de decisión de los pacientes con su enfermedad. Evidentemente se trata de una provocación, en la medida que uno va avanzando en el libro, explica la importancia de la profesión médica ante la nueva complejidad de información y conocimiento ingente. La medicina estratificada o de precisión está empezando y no podemos quedar al margen, la tenemos entre nosotros y debemos preguntarnos si estamos dispuestos a que sea la tecnología la que cambie las organizaciones o si somos nosotros los que tenemos que mandar este cambio desde las propias organizaciones. Personalmente creo que necesitamos aplicarnos seriamente a identificar cuál es el mejor modelo organizativo para la nueva medicina, antes de que la nueva medicina nos haya condicionado a todos. Estamos a tiempo, pero vamos atrasados. Por ahora, soy incapaz de ver ninguna reflexión profunda en este sentido aquí cerca.
Lo que si que podemos hacer hoy es saber dónde estamos, y en qué marco de referencia queremos situarnos. Ya hablé antes de cómo pasamos de las funciones de compra y provisión al marco de la integración asistencial. Ahora conviene entender qué significa el marco de la salud poblacional y cuál es el equipaje necesario para el trayecto. La cuestión fundamental detrás de todo debate de política sanitaria es como lograr un mejor nivel de salud para la población y cómo reducir las diferencias en salud existentes que sean evitables e injustas. Podríamos también llamarlo en términos estadísticos, como aumentar la media y reducir la varianza.
Cuando Stoddart y Kindig definieron el término salud poblacional querían ir más allá de la salud pública convencional. Y precisamente se referían a los resultados de salud de un grupo de personas incluendo la distribución de tales resultados en el grupo. Nos fijamos demasiado en la media y descuidamos la distribución. Ellos enfatizaban especialmente en lo segundo, en como reducir diferencias en salud. Y cual sería la diferencia de la salud poblacional con la salud pública? Mientras la salud pública trata de prevenir epidemias, limitar riesgos ambientales o impulsar comportamientos saludables (prevención y promoción de la salud), en la salud poblacional se parte de la aproximación de salud en todas las políticas para avanzar hacia nuevos instrumentos que tengan impacto real en la población. Hasta aquí uno diría que resulta familiar. En Catalunya por ejemplo el plan interdepartamental e intersectorial de salut pública (PINSAP) pretende precisamente este objetivo, o dentro de él el proyecto Comsalut, pretende orientar orientar el sistema de salut hacia la promoción de la salud y la salud comunitaria. La ejemplaridad del proyecto es indudable del mismo modo que lo es su infradotación de recursos que limita seriamente su impacto en la práctica.
Cuales serían los instrumentos a tener en cuenta para avanzar en la salud poblacional?
Fundamentalmente el punto de partida pasa necesariamente por monitorizar la salud de la población. Hemos basado fundmentalmente los planes de salud en la información de salud percibida a través de las encuestas de salud. La esperanza de vida en buena salud se basa en percepción subjetiva. Ahora bien, necesitamos contrastar si la percepción subjetiva se corresponde con la realidad objetiva de la enfermedad. En un estudio reciente que acabamos de finalizar en Palamós y que se publica en Gaceta Sanitaria mostramos como el 27% de las personas con 2 enfermedades crónicas o con condiciones de salud complejas afirman tener buena salud cuando son encuestados. Es decir informan parcialmente o distorsionadamente de su situación cuando son entrevistadas. Las implicaciones de este resultado son fundamentales para la gestión de la salud poblacional y sobre como las políticas sanitarias descansan sobre un sesgo informativo relevante.
Los registros de morbilidad han mejorado sustancialmente, sin embargo desaprovechamos las oportunidades que ofrece la agregación de información. La estratificación del riesgo a partir de la información de morbilidad es el punto de partida. Es a partir de tal categorización que es posible establecer la modelización predictiva tanto del curso de la enfermedad como de sus costes. En Palamós, una vez más hemos mostrado como una vez conocida la concentración de costes, lo fundamental es predecir la persistencia. Es decir si sabemos el 5% que acumula cerca del 45% del total de costes sanitarios, podemos predecir en qué medida seguiran estando en los siguientes años en este mismo grupo con un área bajo la curva de 0,89 el primer año.
La segunda cuestión es la monitorización de la asistencia. Cuando un médico ve a un paciente, sus resultados se relacionan con la evolución de este paciente o con el grupo de pacientes del médico. Necesitamos medir los episodios de enfermedad, entender como un paciente para un determinado episodio es tratado por distintos profesionales y cual es su resultado en una cohorte dinámica. Necesitamos agregar esta información para conocer el impacto, para mejorar la media y reducir la variación. Kaiser Permanente mostró en el caso de rofecoxib como un medicamento aprobado podía provocar riesgo cardiovascular y muerte y finalmente se retiró del mercado después de que posiblemente sucedieran 28.000 muertes. Esto fue posible por la agregación de información sobre resultados adversos sobre una población de un millón y medio de habitantes. Se vio que los que recibían la dosis máxima de rofecoxib tenían tres veces más probabilidades de sufrir un infarto de miocardio o muerte súbita, en comparación con las personas que habían tomado antiinflamatorios. Otro ejemplo más próximo lo tenemos en el self-audit de la prescripción farmacéutica que puso en marcha Arantxa Catalán en el ICS. La agregación de la información farmacéutica permitió monitorizar pacientes crónicos polimedicados y prevenir efectos adversos. Todo ello empezó hace más de 10 años. En ambos casos no se hablaba de Big Data, pero en el fondo ya se estaba en ello.
La tercera cuestión es la monitorización de los determinantes de la salud. Si admitimos la perspectiva de salud en todas las políticas, necesitamos al mismo tiempo entender cual es el impacto y evolución de las decisiones y acciones sobre entorno físico (mediio ambiente), socioeconómico (educación, empleo, apoyo social y comunitario, vivienda). Pero asimismo convendría establecer programas para la evaluación del genoma poblacional. El ejemplo de Geisinger en Estados Unidos muestra como después de analizar a 200.000 personas, ha sido posible detectar un 4% de población que podía ser susceptible de tratamientos específicos y fundamentados.
La cuarta cuestión es la relativa al comportamiento individual frente a la salud y los riesgos para la salud. Recientemente la OCDE acaba de publicar un manual de instrucciones sobre la cuestión. Bien en realidad, se trata de una aproximación, un intento. Hace más de una década que se habla del pequeño empujón pero sabemos poco de cómo llevarlo a la práctica. Si lo fundamental es definir una arquitectura de elección, en entornos complejos esto resulta casi impracticable. Así pues que debemos estar atentos a lo que funciona y a lo que no. Resumiendo mucho, la salud depende de nuestras decisiones y comportamientos, de factores económicos y sociales, factores físicos y medioambientales, de la asistencia sanitaria y de la genética. ¿Qué parte corresponde a cada uno es compleja de averiguar. Un profesor de Wisconsin, David Kindig al que sigo habitualmente, sitúa el peso de los comportamientos en un 30% del total (decisiones individuales). Y sabemos que incluso, en la genética podemos influir en la medida que nuestros hábitos condicionan también generaciones futuras, la herencia epigenética es fuente de expresión del genoma de nuestros descendientes.
Si el nivel de salud es fruto de todos estos factores que a la vez dependen de cada uno de nosotros y de la colectividad, entonces el paradigma clásico de la producción, donde hay uno que ofrece los servicios -el productor, el sistema de salud- y uno que los recibe - el consumidor- se encuentra en lejos de lo que hay que tener en cuenta a fin de producir más salud.
El compromiso con la propia salud significa tomar decisiones que contribuyen a mantenerla y mejorarla. Hay riesgos que podemos evitar y está a nuestro alcance. La dificultad aparece en la medida en que "somos personas humanas".
La capacidad cognitiva humana viene impulsada por dos "sistemas": (Estos "sistemas" no existen físicamente, pero el modelo funciona bien para explicar y predecir fenómenos!)
- Sistema 1: funciona de forma automática y rápidamente, con poco o ningún esfuerzo y sin sentido de control voluntario (Operaciones automáticas) .La mayoría del tiempo, nuestra capacidad cognitiva viene impulsada por el sistema 1, y de forma bastante eficiente
- Sistema 2: dedica atención actividades mentales que requieren esfuerzo (Operaciones que requieren control). Aparece cuando las decisiones o acciones se vuelven complejas y necesitan atención, con exigencia de «concentración». Es mucho más lento.
Ambos sistemas están activos cuando estamos despiertos.
• El Sistema 1 se ejecuta automáticamente (sin esfuerzo)
• El Sistema 2 se encuentra en modo de bajo esfuerzo, y sólo se utiliza una pequeña parte
• El Sistema 1 genera impresiones, intuiciones, sentimientos, intenciones
• El Sistema 2 en general las acepta
• El Sistema 2 también controla continuamente el comportamiento.
Pero cuando el Sistema 1 se encuentra con una dificultad, pide al Sistema 2 que le ayude:
- Cuando se detecta un problema difícil
- Cuando se detecta algo inesperado o improbable
- El Sistema 1 no se puede detener. Funciona con una heurística determinada y presenta sesgos.
Todo ello puede representar un comportamiento alejado de la racionalidad que el sistema 2 no necesariamente detecte. Una de sus principales características es la pereza, el rechazo a invertir más esfuerzo que el estrictamente necesario. Mientras no se detecta algo raro, se limita a seguir las impresiones del Sistema 1.
Uno de los descubrimientos importantes de los psicólogos cognitivos en las últimas décadas es que cambiar de una tarea a otra representa esfuerzo, y especialmente bajo la presión de la inmediatez. Si así es como funcionamos, entonces las estrategias que presuponen la toma de decisiones racionales entran en contradicción. Siempre se ha pensado desde las estrategias de salud pública que un individuo bien informado, tratará de tomar decisiones que maximicen su beneficio de salud (y en esto se fundamentan las actuaciones en educación sanitaria y difusión de información, necesarias pero no suficientes ).
Las personas humanas tenemos muchos sesgos cognitivos en la toma de decisiones y la economía del comportamiento ha revisado el paradigma convencional del "consumidor racional" que satisface sus intereses, y busca explicar porque somos predictiblemente irracionales. Ante ello considera que es posible diseñar una arquitectura de elección que nos permita superar tales sesgos. Tema controvertido al que no entraré en detalle. En cualquier caso entender el comportamiento individual ante la salud es fundamental incluso antes de hablar de determinantes sociales.
Por lo tanto, somos responsables de nuestra salud en cuanto a decisiones y comportamiento, somos responsables de exponernos a riesgos evitables, al tiempo necesitamos un pequeño empujón (aunque todavía no sabemos como formalizarlo con precisión).
La implicación familiar y comunitaria en la salud se encuentra también en el núcleo de la mejora de la salud. La adquisición de hábitos saludables comienza en la familia. El apoyo y afecto en caso de enfermedad o dependencia contribuye decisivamente. A la economía comportamental le preocupa el gregarismo, herd effect, porque se encuentra en el origen de muchas decisiones por defecto que tomamos. Somos responsables pues de contribuir a crear entornos saludables cercanos y de evitar riesgos extremos.
Precisamente nos encontramos en un contexto que David Courtright ha calificado de capitalismo límbico, en su último libro titulado “The age of addiction”. Explica que las historias de placer, vicio y adicción están relacionadas, y describe los fundametnos de la adicción. El capitalismo límbico se refiere a un entorno económico, tecnológicamente avanzado pero regresivo socialmente en el que las empresas impulsan el consumo excesivo y la adicción. Y esto lo hacen enfocando al sistema límbico, a la parte del cerebro responsable de los sentimientos y la reacción rápida. Es allá donde las neuronas hacen posible el placer, motivación y funciones críticas para la supervivencia. El capitalismo límbico es un producto de la evolución cultural. Otros autores se han referido al mismo fenómeno hablando de determinantes comerciales de la salud. El libro lleva de subtítulo “como los malos hábitos son el origen de un gran negocio”. Y el índice uno ya puede imaginar que repasa alcohol, tabaco, drogas de abuso, alimentos, juego, adicción digital para terminar con una llamada contra los excesos. La sociedad necesita ser capaz de limitar el desarrollo del capitalismo límbico mediante una regulación adecuada. El caso de los opioides en Estados Unidos es desde mi punto de vista un ejemplo claro de capitalismo límbico que además cierra el círculo, crearon la adicción y además generaron negocio fraudulento curándola. Ambos aspectos han sido demostrados. Debemos estar atentos a que no haya contagio próximo de esta epidemia.
La quinta cuestión se refiere a la organización y el talento necesario para mejorar la salud poblacional. Los departamentos de salud pública han estado dirigidos por epidemiólogos. La orientación hacia la salud poblacional requiere multidisciplinariedad, atender a una combinación de capacidades y talento procedente de la Epidemiologia y Medicina, por supuesto, con el Derecho, la Economía, la Política y la Ética. La semana pasada en Catalunya con el impuesto sobre bebidas azucaradas en exceso hubo una acción clara, ante un recurso por defecto de forma se declaró nulo, pero el gobierno volver a aplicar del impuesto subsanando la cuestiones. Los aspectos regulatorios y legales tienen una importancia capital. Entender el impacto en términos del coste-efectividad de las medidas en salud poblacional obliga a análisis que han sido marginales hasta el día de hoy. O los aspectos éticos, igualmente relevantes. La gestión de la salud poblacional necesita permeabilizarse tanto dentro del sistema de salud como fuera y en este sentido hay que conseguir en términos del gobierno, la adecuada interacción que permita la salud en todas las políticas.
He resumido en cinco los aspectos por donde empezar: monitorización de la salud, monitorización de los determinantes de la salud, monitorización de la asistencia y prestaciones, comportamiento individual frente a la salud y los riesgos y la nueva organización para la salud poblacional. Pero hay más cuestiones, por ejemplo una vez resuelta la monitorización cabe pasar a las recomendaciones y la acción.
Kindig, el salubrista que promovió el concepto de salud poblacional, publicó un libro titulado “Purchasing population health” a finales de los 90. Sin duda, desde mi punto de vista lo más desacertado era el título porque enfatizaba una perspectiva mercantilista de la salud totalmente evitable. En realidad el libro y algunos artículos adicionales, se dirigían mostrar que los recursos económicos deberían asignarse con el criterio de mejora de la salud poblacional. Es decir, en lugar de financiar en base a servicios asistenciales recibidos, convendría asignar capitativamente los recursos a una entidad que gestionara la salud poblacional con un indicador último de referencia: la esperanza de vida en buena salud. La idea es sugerente, pero hay una distancia importante para llevarla a la práctica porque desconocemos todavía cuales son los factores que determinan marginalmente el resultado o que lo confunden y cuales son los incentivos que funcionan. Ahora bien, avanzar en la medida de la esperanza de vida en buena salud en areas geográficas pequeñas sería un primer paso.
El reto de la salud poblacional va más allá del sistema de salud y de la política sanitaria. En el parlamento debe confluir en un debate respetuoso, profundo, fundamentado, que busque el consenso y evite la polarización; el gobierno debe captar el mayor talento para una regulación y gestión de la salud poblacional; las organizaciones deben dar respuesta a la atención de calidad con un nuevo marco de referencia; los clínicos deben encajar a la organización guiados por el profesionalismo; los ciudadanos deben asumir la responsabilidad ante su salud y hacer sentir su voz para contribuir a la mejora del sistema.
Hasta aquí pues los mensajes clave que deseaba mostrarles. Esta conferencia ya está publicada en mi blog: econsalut, por si están interesados en revisar su contenido con detalle.
El escritor norteamericano Henry Mencken dijo: “Para cada problema complejo hay una solución que es clara, sencilla y equivocada”. Cambiar hacia un marco de referencia tan complejo como la salud poblacional no puede resolverse con los mensajes de esta conferencia, pero si que espero haberles podido ofrecer pistas claras para que podamos avanzar hacia él.
.
***
Muchas gracias.
Aspectos clave para la mejora de la salud poblacional, una agenda para la acción
Quisiera agradecer en primer lugar la oportunidad de ofrecerles hoy unas reflexiones sobre las cuestiones fundamentales para la mejora de la salud poblacional y algunas pistas para llevarlas a la práctica. La salud y el bienestar de una población toma como punto de referencia inicial la esperanza de vida. Tenemos buenas noticias en este sentido, en Balears en los últimos 15 años, la esperanza de vida ha aumentado una media de 3 años. Para los hombres se sitúa en 80,9 años y para las mujeres en 85,8. Sin embargo, el dato clave es la esperanza de vida en buena salud. Que para los hombres está en 69,2 y en las mujeres en 68,2 (con datos referidos a 2016). Es decir que los hombres pasan el 85% y las mujeres un 79% de la vida en buena salud, es decir en sin limitaciones funcionales o discapacidad. Diez años antes, en 2006, los hombres vivían en buena salud 61 años, un 78% de su vida y las mujeres 60, un 72% de su vida. En 10 años se ha aumentado la vida en buena salud en 7 puntos. Este es un hito dificil de replicar en el futuro porque podemos esperar una tasa marginal de crecimiento más limitada.
Se confirma pues que en la pasada década el mayor aumento se ha producido en los años de vida en buena salud, casi 3 veces más que el aumento de la esperanza de vida al nacer. Este dato debemos recordarlo como fundamental. Interesa la longevidad pero todavía más la calidad de vida en términos marginales. Hasta aquí, he hablado de la media, sin embargo desconocemos como se distribuye este nivel de salud con precisión.
Además convendrá recordar que este cambio ha coincidido en buena parte con la gran recesión económica que hemos vivido. Una situación económica excepcional que en resumen y para referirnos a los mismos años anteriores (2006-2016) la renta per cápita aumentó tan sólo un 3% en Balears. Y además, el nivel de desigualdad económica de las familias se ha agravado como no habíamos conocido nunca en tan poco tiempo. La OCDE ha mostrado que si medimos la desigualdad mediante los cambios en renta disponible, el Estado Español encabeza el conjunto de los 30 países, con un fuerte diferencial. Esta ha sido una situación desconocida para toda nuestra generación que habíamos vivido en un proceso continuado de crecimiento económico. El resultado es que a fecha de hoy el peso de la clase media se ha reducido, mientras que el de las clases bajas ha crecido en la misma proporción. Aun así, la clase media todavía representa el 58% de la población de Balears en 2017.
Es cierto que en unos momentos de cambio económico y social acelerado, el sector salud se vea afectado de forma profunda dada su relevancia en los ciudadanos. Y también es bueno recordar que todos aquellos que anunciaban que el gasto sanitario crecería de forma natural porque la tecnología y el envejecimiento era imparables, es bueno recordarles precisamente que no ha sido así. Hemos tenido envejecimiento en esta década pasada, ha habido innovación tecnológica y hemos conseguido mejorar la esperanza de vida en buena salud con una restricción presupuestaria absoluta, desconocida por muchos de nosotros. Todos los que pregonaban que el gasto era inevitable ahora deberían analizar detenidamente lo que ha sucedido realmente, pero desafortunadamente las dinámicas coyunturales evitan tal reflexión. El gran economista de la salud, Bob Evans, en los años 90 ya había afirmado que la inevitabilidad del gasto sanitario era una falacia, la gran recesión ha tenido la ocasión de confirmarlo.
Conviene reflejar además que la satisfacción ciudadana con el sistema sanitario público se ha mantenido durante estos años. Este es un hecho más que notable, que hay que destacar en un contexto adverso.
Nos encontramos ante un sistema de salud que alcanza unos resultados buenos, más que notables con los recursos que dedicamos. El gran periodista Antoni Bassas decía: Cualquiera que haya ido por el mundo, y no sólo para países más pobres que Cataluña, sino también para países de la Unión Europea, reconocerá que con recortes o sin, en materia de sanidad no sabemos lo que tenemos. Cientos de millones de personas en todo el mundo darían lo que no tienen para poder llevar en el bolsillo una tarjeta que los cubre como nos cubre a nosotros nuestra tarjeta sanitaria.
Estoy convencido de que la mayoría de los que estamos aquí compartimos sus palabras. Entonces, podemos preguntarnos qué justifica que la sanidad sea motivo de tanta controversia, que se nieguen los hechos y que se haga un uso partidista de los argumentos políticos. Esto tiene que ver con varios factores, pero dejadme que en destaque dos: "los medios" y "los marcos de referencia". Vivimos en un tiempo donde la política está secuestrada por lo que Neil Postman tildaba de "show business". Este gran sociólogo escribió en 1985 un libro premonitorio muy recomendable, titulado: "Divertirse hasta morir, el discurso público en la era del show business".
Decía al final del libro: Lo que yo sugiero es lo que decía también Aldous Huxley, estamos en una carrera entre la educación y el desastre, y necesitamos entender la política y la epistemología de los medios de comunicación. Lo que aquejaba a la gente del El mundo feliz no era que estuvieran riendo en lugar de pensar, sino que no sabían de qué estaban riendo y porqué habían dejado de pensar ". Este es un texto escrito antes de la existencia de internet y las redes sociales. No añadiré nada más. La banalización de la cultura y de la política se ha impuesto y nos conviene volver al espíritu crítico fundamentado y al debate respetuoso, aquel que nos hace progresar como sociedad y como personas.
La segunda cuestión que quería destacar proviene de la ciencia cognitiva, en concreto del profesor de Berkeley, George Lakoff y que ahora es conocido por su libro "No pienses en un elefante". Dice: Los marcos de referencia son estructuras mentales que conforman nuestro modo de ver el mundo, conforman los objetivos que nos proponemos, los planes que hacemos, nuestra forma de actuar y lo que cuenta como resultado bueno o malo de nuestras acciones. En política, los marcos conforman nuestras políticas sociales y las instituciones. Cambiar nuestros marcos es cambiar todo esto. Los marcos de referencia no pueden verse ni sentirse, forman parte del inconsciente cognitivo, estructuras de nuestro cerebro a las que no podemos acceder conscientemente, pero que conocemos por sus consecuencias: nuestra forma de pensar y lo que se entiende por sentido común.
Sigo los trabajos de George Lakoff desde hace años y estoy convencido de que nos puede proporcionar la clave para comprender qué está sucediendo en la política y la gestión sanitaria: nos encontramos ante un nuevo marco de referencia que lucha con lo que hemos convivido durante muchos años y que nos mantenía en lo que los psicólogos llaman "zona de confort".
***
Hace tiempo un periodista me preguntaba, me decía Pere, qué crees que necesita el sistema de salud catalán: más financiación o mejor organización?. Yo le dije que la respuesta no era posible lo uno sin lo otro, necesitábamos ambas cosas. Él sin duda quería un titular, y eso ya no cabía. Hay que estar atento a los falsos dilemas y no dejarnos embaucar.
Necesitamos más financiación si somos capaces de demostrar cuál es el valor marginal obtenido de cada euro adicional gastado. De lo contrario me resisto a señalar cuál es el nivel de financiación necesario y cuidadoso. Sin embargo, ya sabemos que el debate sanitario pivota demasiado sobre cuánto dinero nos gastamos y demasiado poco en que obtenemos a cambio. Demasiado en la financiación y poco en la organización.
Por otro lado, hace más de tres décadas que una Constitución dijo que los ciudadanos éramos iguales ante la ley, pero en cambio podemos observar que cuando hay concierto económico, unos ciudadanos pueden gastar en sanidad pública un 40% más que nosotros en el marco de un mismo Estado de Derecho. Lo que tenemos desde entonces es un estado del revés, una chapuza. En un estado del revés nadie puede pensar seriamente en criterios objetivos, ni fijar prioridades, primero hay que ponerlo del derecho. Esto no ha sido posible desde hace muchas, muchas décadas.
Por lo tanto necesitamos mejor financiación en un marco donde podamos priorizar los recursos para alcanzar un valor mayor en salud, y esto sólo será posible en un marco político de referencia nuevo.
***
Pero al mismo tiempo necesitamos mejor organización. Y permítanme una autocita, esta vez del 2001. En un artículo en la revista Fulls Económics del Sistema Sanitari, junto con el amigo Jordi Calsina, escribimos un artículo titulado: "Más allá de la separación de funciones: las organizaciones sanitarias integradas ". Hace dieciocho años que algunos ya nos habíamos dado cuenta de que había que cambiar de marco de referencia en el aspecto organizativo. Han pasado años y nos hemos mantenido en una "zona de confort". Había que ir más allá de la separación de funciones para que algunos vemos que era un concepto difuso, complicado de llevar a cabo en la práctica en un entorno donde la transferencia de riesgo sólo se sostiene sobre el papel. Y proponíamos las organizaciones sanitarias integradas en la medida que cambiaba la lógica de la compra de servicios por el compromiso con la salud de la comunidad por parte de todos los proveedores.
He estado siguiendo y todavía sigo de cerca el esfuerzo hecho desde Palamós por los Servicios Sanitarios Integrados del Baix Empordà, enfocado hacia una visión de servicio integradora. No es por casualidad que un residente distinguido como el novelista Tom Sharpe escribía con claridad en The Guardian sobre la calidad de servicio que recibió y consideraba que nunca el NHS lo hubiera tratado igual. Más allá de esta anécdota, si me preguntaran por un modelo organizativo apropiado sería este, evidentemente como siempre mejorable.
Tenemos un sistema público de salud con unas características organizativas singulares destacables, citaré dos solamente. La primera es la planificación de recursos, el mapa sanitario, la condición previa a cualquier desbarajuste inversor y al exceso de capacidad instalada que suele suceder en entornos privados. La segunda es la inexistencia del pago por acto médico, motivo de fragmentación, sobrediagnóstico y exceso de tratamiento a muchos sistemas de salud. Aquellos que aún lo aplican luchan por una alternativa.
Ahora bien, el ejercicio responsable de la gobernanza de las organizaciones ha sido posiblemente la pieza más olvidada del engranaje del sistema público de salud. Algunas de las controversias del momento nos las hubiéramos podido ahorrar si hubiéramos dedicado más esfuerzos a estructurar la función de gobierno. Como siempre generalizar tiene riesgos, y por lo tanto ha habido casos ejemplares de gobernanza pero que en mi opinión han sido aislados.
***
Y llegados hasta aquí, hay que recordar las singularidades del entorno de la gestión sanitaria. En Jeffrey Harris, economista y médico, profesor del MIT y internista al Hospital General de Massachussets escribió en 1977 un extraordinario artículo titulado: "La organización interna de los hospitales, algunas implicaciones económicas". Tengo que confesar que fue uno de los primeros artículos de economía de la salud que leí y que me impactó. Pero no sólo a mí, es uno de los artículos más referenciados que hay a fecha de hoy. Esencialmente en Jeffrey Harris dijo en otras palabras, algunas cosas que sabemos los que hemos sido gerentes de hospital. Él sugería que el hospital en realidad son dos empresas: la administrativa y la médica. En esta organización dual hay un conjunto de reglas implícitas de asignación de recursos. La controversia se produce cuando la demanda médica supera la capacidad ofrecida por la administrativa. Nos enfocamos demasiado a analizar la parte administrativa y no tanto a la médica. Y terminaba señalando que hay una nueva organización interna de los hospitales.
Ahora si tuviera que reescribir el artículo seguro que iría más allá de los hospitales y pensaría en organizaciones sanitarias integradas. Considero que Harris acertó en el diagnóstico pero se quedó corto en la terapia, se quedó a medias. Hay que repensar muy seriamente la posición de los médicos dentro de la organización sanitaria. Estoy convencido de que el encaje actual chirría, y las propuestas para avanzar son limitadas. Después de observar modelos alternativos, he llegado al convencimiento de que la relación laboral de la profesión médica en un convenio colectivo difícilmente encaja con la realidad de la tarea, el talento y los resultados que se esperan. Si dentro de la relación laboral tengo dudas, imaginen los que tendré si hay una atribución funcionarial vitalicia, en propiedad, como lo llaman. A fecha de hoy todavía tengo pendiente de encontrar a alguien que me justifique que un médico debe ser funcionario con un argumento convincente.
Para enfocar una visión alternativa, es necesario comprender la profesión médica en el marco organizativo del sistema de salud con las coordenadas inherentes del profesionalismo.
Hay que ser precisos en lo que estamos hablando. Entiendo el profesionalismo más allá de la autonomía estricta y sesgada que algunos defienden. Para profesionalismo quiero decir: (1) altruismo, en caso de conflicto de interés entre intereses profesionales y los de los pacientes, hay que decantarse en favor de los pacientes, (2) un compromiso en la mejora, los profesionales deben actualizarse en el nuevo conocimiento y su incorporación a la práctica (3) revisión entre colegas, los médicos deben ser capaces de supervisar el trabajo de los colegas, para proteger a los pacientes y (4) los médicos deben incorporar el criterio de eficiencia social en las decisiones clínicas.
Si pensamos en una integración asistencial exitosa, necesitamos que la coordinación y motivación en el ámbito clínico sea máxima. En la actualidad, muchos de los avances obtenidos han tenido relación con la capacidad de liderazgo y la cultura organizativa, aunque los incentivos explícitos han sido escasos. La prueba definitiva de que puede llegar más allá en la integración es cuando los profesionales se implican porque más allá de los atributos del profesionalismo, sienten que su esfuerzo se ve compensado y respetado. Muy a menudo, la segunda cuestión toma más importancia que la primera, quiero decir que el respeto ocupa una posición superior a la compensación material. Valorar el trabajo bien hecho, reconocerlo, es fundamental en el entorno profesional. En esto, la sociedad profesional es capaz de hacerlo mejor que tal como lo hace la parte administrativa de la organización hoy en día.
***
Estamos asistiendo a un cambio profundo en la "función de producción de salud". En el libro del cardiólogo Eric Topol titulado "El paciente te atenderá", quiere señalar las nuevas capacidades de decisión de los pacientes con su enfermedad. Evidentemente se trata de una provocación, en la medida que uno va avanzando en el libro, explica la importancia de la profesión médica ante la nueva complejidad de información y conocimiento ingente. La medicina estratificada o de precisión está empezando y no podemos quedar al margen, la tenemos entre nosotros y debemos preguntarnos si estamos dispuestos a que sea la tecnología la que cambie las organizaciones o si somos nosotros los que tenemos que mandar este cambio desde las propias organizaciones. Personalmente creo que necesitamos aplicarnos seriamente a identificar cuál es el mejor modelo organizativo para la nueva medicina, antes de que la nueva medicina nos haya condicionado a todos. Estamos a tiempo, pero vamos atrasados. Por ahora, soy incapaz de ver ninguna reflexión profunda en este sentido aquí cerca.
Lo que si que podemos hacer hoy es saber dónde estamos, y en qué marco de referencia queremos situarnos. Ya hablé antes de cómo pasamos de las funciones de compra y provisión al marco de la integración asistencial. Ahora conviene entender qué significa el marco de la salud poblacional y cuál es el equipaje necesario para el trayecto. La cuestión fundamental detrás de todo debate de política sanitaria es como lograr un mejor nivel de salud para la población y cómo reducir las diferencias en salud existentes que sean evitables e injustas. Podríamos también llamarlo en términos estadísticos, como aumentar la media y reducir la varianza.
Cuando Stoddart y Kindig definieron el término salud poblacional querían ir más allá de la salud pública convencional. Y precisamente se referían a los resultados de salud de un grupo de personas incluendo la distribución de tales resultados en el grupo. Nos fijamos demasiado en la media y descuidamos la distribución. Ellos enfatizaban especialmente en lo segundo, en como reducir diferencias en salud. Y cual sería la diferencia de la salud poblacional con la salud pública? Mientras la salud pública trata de prevenir epidemias, limitar riesgos ambientales o impulsar comportamientos saludables (prevención y promoción de la salud), en la salud poblacional se parte de la aproximación de salud en todas las políticas para avanzar hacia nuevos instrumentos que tengan impacto real en la población. Hasta aquí uno diría que resulta familiar. En Catalunya por ejemplo el plan interdepartamental e intersectorial de salut pública (PINSAP) pretende precisamente este objetivo, o dentro de él el proyecto Comsalut, pretende orientar orientar el sistema de salut hacia la promoción de la salud y la salud comunitaria. La ejemplaridad del proyecto es indudable del mismo modo que lo es su infradotación de recursos que limita seriamente su impacto en la práctica.
Cuales serían los instrumentos a tener en cuenta para avanzar en la salud poblacional?
Fundamentalmente el punto de partida pasa necesariamente por monitorizar la salud de la población. Hemos basado fundmentalmente los planes de salud en la información de salud percibida a través de las encuestas de salud. La esperanza de vida en buena salud se basa en percepción subjetiva. Ahora bien, necesitamos contrastar si la percepción subjetiva se corresponde con la realidad objetiva de la enfermedad. En un estudio reciente que acabamos de finalizar en Palamós y que se publica en Gaceta Sanitaria mostramos como el 27% de las personas con 2 enfermedades crónicas o con condiciones de salud complejas afirman tener buena salud cuando son encuestados. Es decir informan parcialmente o distorsionadamente de su situación cuando son entrevistadas. Las implicaciones de este resultado son fundamentales para la gestión de la salud poblacional y sobre como las políticas sanitarias descansan sobre un sesgo informativo relevante.
Los registros de morbilidad han mejorado sustancialmente, sin embargo desaprovechamos las oportunidades que ofrece la agregación de información. La estratificación del riesgo a partir de la información de morbilidad es el punto de partida. Es a partir de tal categorización que es posible establecer la modelización predictiva tanto del curso de la enfermedad como de sus costes. En Palamós, una vez más hemos mostrado como una vez conocida la concentración de costes, lo fundamental es predecir la persistencia. Es decir si sabemos el 5% que acumula cerca del 45% del total de costes sanitarios, podemos predecir en qué medida seguiran estando en los siguientes años en este mismo grupo con un área bajo la curva de 0,89 el primer año.
La segunda cuestión es la monitorización de la asistencia. Cuando un médico ve a un paciente, sus resultados se relacionan con la evolución de este paciente o con el grupo de pacientes del médico. Necesitamos medir los episodios de enfermedad, entender como un paciente para un determinado episodio es tratado por distintos profesionales y cual es su resultado en una cohorte dinámica. Necesitamos agregar esta información para conocer el impacto, para mejorar la media y reducir la variación. Kaiser Permanente mostró en el caso de rofecoxib como un medicamento aprobado podía provocar riesgo cardiovascular y muerte y finalmente se retiró del mercado después de que posiblemente sucedieran 28.000 muertes. Esto fue posible por la agregación de información sobre resultados adversos sobre una población de un millón y medio de habitantes. Se vio que los que recibían la dosis máxima de rofecoxib tenían tres veces más probabilidades de sufrir un infarto de miocardio o muerte súbita, en comparación con las personas que habían tomado antiinflamatorios. Otro ejemplo más próximo lo tenemos en el self-audit de la prescripción farmacéutica que puso en marcha Arantxa Catalán en el ICS. La agregación de la información farmacéutica permitió monitorizar pacientes crónicos polimedicados y prevenir efectos adversos. Todo ello empezó hace más de 10 años. En ambos casos no se hablaba de Big Data, pero en el fondo ya se estaba en ello.
La tercera cuestión es la monitorización de los determinantes de la salud. Si admitimos la perspectiva de salud en todas las políticas, necesitamos al mismo tiempo entender cual es el impacto y evolución de las decisiones y acciones sobre entorno físico (mediio ambiente), socioeconómico (educación, empleo, apoyo social y comunitario, vivienda). Pero asimismo convendría establecer programas para la evaluación del genoma poblacional. El ejemplo de Geisinger en Estados Unidos muestra como después de analizar a 200.000 personas, ha sido posible detectar un 4% de población que podía ser susceptible de tratamientos específicos y fundamentados.
La cuarta cuestión es la relativa al comportamiento individual frente a la salud y los riesgos para la salud. Recientemente la OCDE acaba de publicar un manual de instrucciones sobre la cuestión. Bien en realidad, se trata de una aproximación, un intento. Hace más de una década que se habla del pequeño empujón pero sabemos poco de cómo llevarlo a la práctica. Si lo fundamental es definir una arquitectura de elección, en entornos complejos esto resulta casi impracticable. Así pues que debemos estar atentos a lo que funciona y a lo que no. Resumiendo mucho, la salud depende de nuestras decisiones y comportamientos, de factores económicos y sociales, factores físicos y medioambientales, de la asistencia sanitaria y de la genética. ¿Qué parte corresponde a cada uno es compleja de averiguar. Un profesor de Wisconsin, David Kindig al que sigo habitualmente, sitúa el peso de los comportamientos en un 30% del total (decisiones individuales). Y sabemos que incluso, en la genética podemos influir en la medida que nuestros hábitos condicionan también generaciones futuras, la herencia epigenética es fuente de expresión del genoma de nuestros descendientes.
Si el nivel de salud es fruto de todos estos factores que a la vez dependen de cada uno de nosotros y de la colectividad, entonces el paradigma clásico de la producción, donde hay uno que ofrece los servicios -el productor, el sistema de salud- y uno que los recibe - el consumidor- se encuentra en lejos de lo que hay que tener en cuenta a fin de producir más salud.
El compromiso con la propia salud significa tomar decisiones que contribuyen a mantenerla y mejorarla. Hay riesgos que podemos evitar y está a nuestro alcance. La dificultad aparece en la medida en que "somos personas humanas".
La capacidad cognitiva humana viene impulsada por dos "sistemas": (Estos "sistemas" no existen físicamente, pero el modelo funciona bien para explicar y predecir fenómenos!)
- Sistema 1: funciona de forma automática y rápidamente, con poco o ningún esfuerzo y sin sentido de control voluntario (Operaciones automáticas) .La mayoría del tiempo, nuestra capacidad cognitiva viene impulsada por el sistema 1, y de forma bastante eficiente
- Sistema 2: dedica atención actividades mentales que requieren esfuerzo (Operaciones que requieren control). Aparece cuando las decisiones o acciones se vuelven complejas y necesitan atención, con exigencia de «concentración». Es mucho más lento.
Ambos sistemas están activos cuando estamos despiertos.
• El Sistema 1 se ejecuta automáticamente (sin esfuerzo)
• El Sistema 2 se encuentra en modo de bajo esfuerzo, y sólo se utiliza una pequeña parte
• El Sistema 1 genera impresiones, intuiciones, sentimientos, intenciones
• El Sistema 2 en general las acepta
• El Sistema 2 también controla continuamente el comportamiento.
Pero cuando el Sistema 1 se encuentra con una dificultad, pide al Sistema 2 que le ayude:
- Cuando se detecta un problema difícil
- Cuando se detecta algo inesperado o improbable
- El Sistema 1 no se puede detener. Funciona con una heurística determinada y presenta sesgos.
Todo ello puede representar un comportamiento alejado de la racionalidad que el sistema 2 no necesariamente detecte. Una de sus principales características es la pereza, el rechazo a invertir más esfuerzo que el estrictamente necesario. Mientras no se detecta algo raro, se limita a seguir las impresiones del Sistema 1.
Uno de los descubrimientos importantes de los psicólogos cognitivos en las últimas décadas es que cambiar de una tarea a otra representa esfuerzo, y especialmente bajo la presión de la inmediatez. Si así es como funcionamos, entonces las estrategias que presuponen la toma de decisiones racionales entran en contradicción. Siempre se ha pensado desde las estrategias de salud pública que un individuo bien informado, tratará de tomar decisiones que maximicen su beneficio de salud (y en esto se fundamentan las actuaciones en educación sanitaria y difusión de información, necesarias pero no suficientes ).
Las personas humanas tenemos muchos sesgos cognitivos en la toma de decisiones y la economía del comportamiento ha revisado el paradigma convencional del "consumidor racional" que satisface sus intereses, y busca explicar porque somos predictiblemente irracionales. Ante ello considera que es posible diseñar una arquitectura de elección que nos permita superar tales sesgos. Tema controvertido al que no entraré en detalle. En cualquier caso entender el comportamiento individual ante la salud es fundamental incluso antes de hablar de determinantes sociales.
Por lo tanto, somos responsables de nuestra salud en cuanto a decisiones y comportamiento, somos responsables de exponernos a riesgos evitables, al tiempo necesitamos un pequeño empujón (aunque todavía no sabemos como formalizarlo con precisión).
La implicación familiar y comunitaria en la salud se encuentra también en el núcleo de la mejora de la salud. La adquisición de hábitos saludables comienza en la familia. El apoyo y afecto en caso de enfermedad o dependencia contribuye decisivamente. A la economía comportamental le preocupa el gregarismo, herd effect, porque se encuentra en el origen de muchas decisiones por defecto que tomamos. Somos responsables pues de contribuir a crear entornos saludables cercanos y de evitar riesgos extremos.
Precisamente nos encontramos en un contexto que David Courtright ha calificado de capitalismo límbico, en su último libro titulado “The age of addiction”. Explica que las historias de placer, vicio y adicción están relacionadas, y describe los fundametnos de la adicción. El capitalismo límbico se refiere a un entorno económico, tecnológicamente avanzado pero regresivo socialmente en el que las empresas impulsan el consumo excesivo y la adicción. Y esto lo hacen enfocando al sistema límbico, a la parte del cerebro responsable de los sentimientos y la reacción rápida. Es allá donde las neuronas hacen posible el placer, motivación y funciones críticas para la supervivencia. El capitalismo límbico es un producto de la evolución cultural. Otros autores se han referido al mismo fenómeno hablando de determinantes comerciales de la salud. El libro lleva de subtítulo “como los malos hábitos son el origen de un gran negocio”. Y el índice uno ya puede imaginar que repasa alcohol, tabaco, drogas de abuso, alimentos, juego, adicción digital para terminar con una llamada contra los excesos. La sociedad necesita ser capaz de limitar el desarrollo del capitalismo límbico mediante una regulación adecuada. El caso de los opioides en Estados Unidos es desde mi punto de vista un ejemplo claro de capitalismo límbico que además cierra el círculo, crearon la adicción y además generaron negocio fraudulento curándola. Ambos aspectos han sido demostrados. Debemos estar atentos a que no haya contagio próximo de esta epidemia.
La quinta cuestión se refiere a la organización y el talento necesario para mejorar la salud poblacional. Los departamentos de salud pública han estado dirigidos por epidemiólogos. La orientación hacia la salud poblacional requiere multidisciplinariedad, atender a una combinación de capacidades y talento procedente de la Epidemiologia y Medicina, por supuesto, con el Derecho, la Economía, la Política y la Ética. La semana pasada en Catalunya con el impuesto sobre bebidas azucaradas en exceso hubo una acción clara, ante un recurso por defecto de forma se declaró nulo, pero el gobierno volver a aplicar del impuesto subsanando la cuestiones. Los aspectos regulatorios y legales tienen una importancia capital. Entender el impacto en términos del coste-efectividad de las medidas en salud poblacional obliga a análisis que han sido marginales hasta el día de hoy. O los aspectos éticos, igualmente relevantes. La gestión de la salud poblacional necesita permeabilizarse tanto dentro del sistema de salud como fuera y en este sentido hay que conseguir en términos del gobierno, la adecuada interacción que permita la salud en todas las políticas.
He resumido en cinco los aspectos por donde empezar: monitorización de la salud, monitorización de los determinantes de la salud, monitorización de la asistencia y prestaciones, comportamiento individual frente a la salud y los riesgos y la nueva organización para la salud poblacional. Pero hay más cuestiones, por ejemplo una vez resuelta la monitorización cabe pasar a las recomendaciones y la acción.
Kindig, el salubrista que promovió el concepto de salud poblacional, publicó un libro titulado “Purchasing population health” a finales de los 90. Sin duda, desde mi punto de vista lo más desacertado era el título porque enfatizaba una perspectiva mercantilista de la salud totalmente evitable. En realidad el libro y algunos artículos adicionales, se dirigían mostrar que los recursos económicos deberían asignarse con el criterio de mejora de la salud poblacional. Es decir, en lugar de financiar en base a servicios asistenciales recibidos, convendría asignar capitativamente los recursos a una entidad que gestionara la salud poblacional con un indicador último de referencia: la esperanza de vida en buena salud. La idea es sugerente, pero hay una distancia importante para llevarla a la práctica porque desconocemos todavía cuales son los factores que determinan marginalmente el resultado o que lo confunden y cuales son los incentivos que funcionan. Ahora bien, avanzar en la medida de la esperanza de vida en buena salud en areas geográficas pequeñas sería un primer paso.
El reto de la salud poblacional va más allá del sistema de salud y de la política sanitaria. En el parlamento debe confluir en un debate respetuoso, profundo, fundamentado, que busque el consenso y evite la polarización; el gobierno debe captar el mayor talento para una regulación y gestión de la salud poblacional; las organizaciones deben dar respuesta a la atención de calidad con un nuevo marco de referencia; los clínicos deben encajar a la organización guiados por el profesionalismo; los ciudadanos deben asumir la responsabilidad ante su salud y hacer sentir su voz para contribuir a la mejora del sistema.
Hasta aquí pues los mensajes clave que deseaba mostrarles. Esta conferencia ya está publicada en mi blog: econsalut, por si están interesados en revisar su contenido con detalle.
El escritor norteamericano Henry Mencken dijo: “Para cada problema complejo hay una solución que es clara, sencilla y equivocada”. Cambiar hacia un marco de referencia tan complejo como la salud poblacional no puede resolverse con los mensajes de esta conferencia, pero si que espero haberles podido ofrecer pistas claras para que podamos avanzar hacia él.
.
***
Muchas gracias.
El pi de Formentor
Subscriure's a:
Missatges (Atom)





.jpg)




















