How A.I. Is Humanizing Healthcare with Dr. Eric Topol
Can A.I. and machine learning make healthcare more humane, loving, and passionate?
Dr. Eric Topol thinks so.
Dr. Topol (Website | Twitter) is a geneticist, medical researcher, and author of Deep Medicine. He has written over 1100 peer-reviewed articles and is one of the top most-cited medical researchers in the world.
In this episode, Chad sits down with Dr. Topol to talk about how A.I. and machine learning are putting the patient experience back at the forefront of healthcare. Dr. Topol also explains why you don’t actually own your own medical data and what steps we need to take to get it back.
17 d’abril 2019
09 d’abril 2019
A lifetime fair drug pricing system
When Is The Price Of A Drug Unjust? The Average Lifetime Earnings Standard
Is there any measure for unfair pricing in drugs?. According to Ezequiel Emanuel prices should not
Is there any measure for unfair pricing in drugs?. According to Ezequiel Emanuel prices should not
"exceed 11 percent of the average American’s disposable income. This suggests that current prices for many drugs are excessive and unjust."Why?.
Currently, average lifetime costs for health care are estimated at 31 percent of disposable income. Drugs account for 17 percent of health care expenses. A threshold for medical care as a share of disposable income that is set 10 percentage points higher than the current average amount spent on medical care (at 41 percent, or $261,907) is generous, as is a threshold for drug costs as a share of medical costs set 10 percentage points higher (at 27 percent, or $70,715) than the current share. Using these standards, the costs for all of the drugs a person takes in a lifetime should not consume more than 27 percent of medical costs, or $70,715. This constitutes 11 percent of lifetime disposable income.He achieves this conclusion after applying these principles:
1. Complete life. The unit of analysis should not be a year or other limited time frame, but rather the impact over a whole lifetimeThis article represents a deep change of perspective on drug pricing. Cost-effectiveness of individual drugs are not enough, a lifetime and societal perspective is necessary. I agree in this part, however methodological implications are huge and uncertain.
2. Limited resources. The just price of a drug should reserve enough resources for people to pursue valuable life activities
3. Value. There should exist a close relationship between the actual benefits of an intervention and its price
4. Comprehensiveness. Life activities other than health matter; in considering the benefits of a treatment, we should also consider how it affects education, employment, and other valuable life activities
Bonnard at Tate modern right now
05 d’abril 2019
Personal Health Data Cooperatives
Personal Data Cooperatives – A New Data Governance Framework for Data Donation and Precision Health
The Ethics of Medical Data Donation
The Ethics of Medical Data Donation
Given that personal data can be copied, individuals are entitled to copies of their data and individuals are the ultimate aggregators of all their personal data, citizens are elevated to new roles at the center of health research and a novel personal data economy. There, citizens, not some multinational company, control the use of and benefit from the intellectual and economic value of these data.In a chapter of the book you'll find a description of MIDATA cooperative, a swiss case. My impression is that this is the appropriate approach. A closer initiative is SalusCoop. However, as happens in any public good, its governance is always the foremost issue.
03 d’abril 2019
01 d’abril 2019
30 de març 2019
Medicine as a data science (6)
Adapting to Artificial Intelligence: Radiologists and Pathologists as Information Specialists
While some physicians are lobbying for creating more specialties, Jah and Topol argue exactly the opposite. Radiology, pathology and in vitro diagnostics should be under the same umbrella: "the information specialists":
While some physicians are lobbying for creating more specialties, Jah and Topol argue exactly the opposite. Radiology, pathology and in vitro diagnostics should be under the same umbrella: "the information specialists":
Because pathology and radiology have a similar past and a common destiny,
perhaps these specialties should be mergedinto a single entity, the “information specialist,” whose responsibility will not be so much to extract information from images and histology but to manage the information extracted by artificial intelligence in the clinical context of the patient.
There may be resistance to merging 2 distinct medical specialties, each of which has unique pedagogy, tradition, accreditation,and reimbursement.However, artificial intelligence will change these diagnostic fields. The merger is a natural fusion of human talent and artificial intelligence. United, radiologists and pathologists can thrive with the rise of artificial intelligence.
The history of automation in the broader economy has a reassuring message. Jobs are not lost; rather, roles are redefined; humans are displaced to tasks needing a human element. Radiologists and pathologists need not fear artificial intelligence but rather must adapt incrementally to artificial intelligence, retaining their own services for cognitively challenging tasks.A unified discipline, information specialists would best be able to captain artificial intelligence and guide medical information to improve patient care.You may agree or not. Technology is breaking barriers and creating bridges. Food for thought.
Josep Segú - Brooklyn Bridge
27 de març 2019
The deep side of medicine and the gift of time
Deep Medicine
Nowadays the impact of Artificial Intelligence in Medicine is unknown. Every other day you may hear about robots and how they will replace humans. Nobody knows about it, distrust charlatans. The only thing that is real is what is already happening. Eric Topol has tried to do this in his new book Deep Medicine. But at the same time he considers that AI will let physicians humanise medicine, "the gift of time", and says:
The remaining elements of the book are of interest to explain the current state of advances in apps and tools for clinical decision making. You'll find helpful information and a great summary of AI in medicine. However, my suggestion is that you can forget the subtitle of the book: "How artificial intelligence can make healthcare human again". It's naïve.
Nowadays the impact of Artificial Intelligence in Medicine is unknown. Every other day you may hear about robots and how they will replace humans. Nobody knows about it, distrust charlatans. The only thing that is real is what is already happening. Eric Topol has tried to do this in his new book Deep Medicine. But at the same time he considers that AI will let physicians humanise medicine, "the gift of time", and says:
"As machines get smarter, humans will need to evolve along a different path from machines and become more humane"This may be Eric Topol's desire, nothing to add. My view is quite different. I'm not sure about the contribution of AI to a humanised medicine . This has to do with professionalism, not with AI. And the incentives for professionalism are plunging, while commercialism is on the rise. This is the key issue.
The remaining elements of the book are of interest to explain the current state of advances in apps and tools for clinical decision making. You'll find helpful information and a great summary of AI in medicine. However, my suggestion is that you can forget the subtitle of the book: "How artificial intelligence can make healthcare human again". It's naïve.
22 de març 2019
The Theranos contretemps as a serious scandal (2)
The DropoutPodcast by ABC Radio & ABC News Nightline
The inventor
Now you can hear the ABC radio podcast in 6 chapters on Theranos scandal. Report at The Verge. Highly recommended.
And the HBO new documentary explains all the details in 2 hours. The trailer:
The inventor
Now you can hear the ABC radio podcast in 6 chapters on Theranos scandal. Report at The Verge. Highly recommended.
And the HBO new documentary explains all the details in 2 hours. The trailer:
20 de març 2019
#CRISPRWHO: notes on a new scandal
Open AccessOpen Access license
#CRISPRbabies: Notes on a ScandalThis week:
An advisory panel to the World Health Organization has called for the creation of a global registry to monitor gene-editing research in humans, the organization announced yesterday (March 19). The recommendations of the 18-person committee, which was established following news late last year that Chinese scientist He Jiankui had carried out human gene editing in secret, are aimed at improving transparency and responsibility in the field, the announcement says.
The panel’s advice did not go so far as to call for a moratorium on all human germline editing, unlike some other groups. Last week, a group of scientists and bioethicists from seven countries penned a commentary in Nature that argued for “a fixed period during which no clinical uses of germline editing whatsoever are allowed.” Such a moratorium would allow time for ethical and moral debate and for the agreement of an international regulatory framework, they wrote.After the initial #CRISPRbabies scandal , we are facing a new one. The WHO pannel is asking for a registry instead of a moratorium. The battle has finished. Game over. From now on, the human being will be affected from such decision. One of the worst decisions in the human history.
17 de març 2019
Improving the pharmaceutical regulation production function
Using Routinely Collected Data to Inform Pharmaceutical Policies
With the broadening of data available for officials to regulate markets, things could change. The issue is specially relevant for pharmaceuticals. Up to now if you want information about the market you have to use IMS data. Now governments that pay the drugs bill can use their own data to improve regulation. Better knowledge could represent better regulation if it is performed appropriately and on a timely basis. The OECD report tries to put all these elements together and highlight the opportunities ahead.
With the broadening of data available for officials to regulate markets, things could change. The issue is specially relevant for pharmaceuticals. Up to now if you want information about the market you have to use IMS data. Now governments that pay the drugs bill can use their own data to improve regulation. Better knowledge could represent better regulation if it is performed appropriately and on a timely basis. The OECD report tries to put all these elements together and highlight the opportunities ahead.
This report provides an overview of patient-level data on medicines routinely collected in health systems from administrative sources, e.g. pharmacy records, electronic health records and insurance claims. In total 26 OECD and EU member countries responded to a survey addressing the availability and accessibility of routinely collected data on medicines and their applicability to developing evidence. The report further explores the utility of evidence from clinical practice, looking at experiences and initiatives across the OECD and EU.Governments will have to improve big data capabilities and add new talent.
08 de març 2019
Never ending health reforms
Reformas pendientes en la organización de la actividad sanitaria
A new issue of Cuadernos ICE shows the current state of the health system. You'll find an article that explains the main constraints to be overcome with all the details. Above all, in my opinion is the quality of institutions. The remaining articles are highly recommended as well.
We are living on a slippery slope and nobody cares about it, it seems that key decision makers have forgotten to read and accept facts as they are. I strongly suggest a reading of these articles. Something should be done to avoid having to rewrite the same a decade later, as it has happened. Maybe the reforms never end because they still have to start.
Take a chance, play your part. Don't wait too long.
PS. Facts (1) and (2)
A new issue of Cuadernos ICE shows the current state of the health system. You'll find an article that explains the main constraints to be overcome with all the details. Above all, in my opinion is the quality of institutions. The remaining articles are highly recommended as well.
We are living on a slippery slope and nobody cares about it, it seems that key decision makers have forgotten to read and accept facts as they are. I strongly suggest a reading of these articles. Something should be done to avoid having to rewrite the same a decade later, as it has happened. Maybe the reforms never end because they still have to start.
Take a chance, play your part. Don't wait too long.
PS. Facts (1) and (2)
You can cry a million tears
You can wait a million years
If you think that time will change your ways
Don't wait too long
When your morning turns to night
Who'll be loving you by candlelight
If you think that time will change your ways
Don't wait too long
Maybe I got a lot to learn
Time can slip away
Sometimes you got to lose it all
Before you find your way
Take a chance, play your part
Make romance, it might brake your heart
But if you think that time will change your ways
Don't wait too long
It may rain, it may shine
Love will age like fine red wine
But if you think that time will change your ways
Don't wait too long
Maybe you and I got a lot to learn
Don't waste another day
Maybe you got to lose it all
Before you find your way
Take a chance, play your part
Make romance, it might break your heart
But if you think that time will change your ways
Don't wait too long
Don't wait
Hmm... Don't wait
07 de març 2019
Revisiting the economic foundations of health insurance
Choose to Lose: Health Plan Choices from a Menu with Dominated Option
We know that more choice is not always better. Former posts have emphasized this issue. Loewenstein et al. provide remarkable evidence of what happens with health insurance:
PS. G. Loeweinstein will be in Barcelona next week at Barcelona Jocs.
We know that more choice is not always better. Former posts have emphasized this issue. Loewenstein et al. provide remarkable evidence of what happens with health insurance:
Our findings offer perhaps the strongest evidence to date that insurance reveal as much or more about consumer understanding than about actual health-related risk preferences. In this sense, our setting provides a rare opportunity to conduct a specification check on
the standard insurance demand model absent search frictions.
Our findings challenge the standard practice of inferring risk preferences from insurance choices and raise doubts about the welfare benefits of health reforms that expand consumer choice.If this is so, many books should be rewritten asap.
PS. G. Loeweinstein will be in Barcelona next week at Barcelona Jocs.
04 de març 2019
Pharma landscape
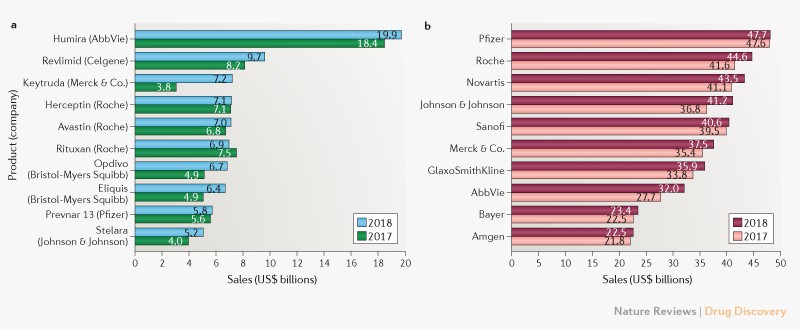
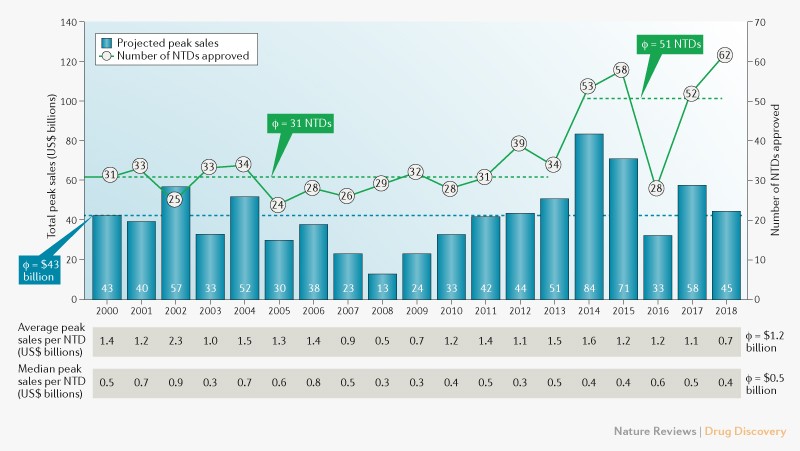
The Global Use of Medicine in 2019 and Outlook to 2023
The summary of IQVIA report:
The summary of IQVIA report:
- Global spending on medicines reached $1.2 trillion in 2018 and is set to exceed $1.5 trillion by 2023.
- Invoice spending in the United States is expected to grow at 4– 7% to $625–655 billion across all channels, but net manufacturer revenue is expected to be 35% below invoice and have growth of 3-6% as price growth slows on both an invoice and net basis.
- Net drug prices in the United States increased at an estimated 1.5% in 2018 and are expected to rise at 0–3% over the next five years.
- China reached $137 billion in medicine spending in 2018, but will see growth slow to 3-6% in the next five years as central government reforms to expand insurance access to both rural and urban residents, as well as expansions and modernizations of the hospital system and primary care services have been largely achieved and efforts shift to cost optimization and addressing corruption.
- Medicine spending in Japan totaled $86 billion in 2018, however spending on medicines is expected to decline from -3 to 0% through 2023, due to the effect of exchange rates and continued uptake of generics and offset by the uptake of new products.
- The number of new products launched is expected to increase from an average of 46 in the past five years to 54 through 2023, and the average spending in developed markets on new brands is expected to rise slightly to $45.8 billion in the next five years, but represent a smaller share of brand spending
01 de març 2019
Rescuing citizens from the "rule of rescue"
People feel a need to rescue identifiable individuals facing avoidable death or harm. This is a well known fact explained in 1968 by the Nobel laureate Thomas Schelling from an economic perspective and by Jonsen in the bioethics context in 1986.
Just to finish, check this final fact:
"A single death is a tragedy; a million deaths is a statistic." This quote reflects exactly what we are talking about. However, the issue is: Do you accept the rescue at any price with public money?
These previous posts of this blog: (1) and (2) explain the details. I'll not insist on what I've already said. I suggest you have a look at them.
Today you can asess these three facts:
1. A country spends 38m € in drugs for 249 patients in 2018. A lifetime treatment.
2. A country has a waiting list of 132.025 patients for surgery, 123.249 patients for diagnostic tests, and 424.715 patients waiting for a visit to the specialist. Total people waiting: 679.989 patients in a country with 7.543.825 inhabitants. 9% of the population is in the waiting list for a health service. However, 25% have voluntary duplicate insurance and could jump the list. Therefore the exact figure is 12% of inhabitants waiting.
3. A country knows that spending 10m € in addition every year can increase cardiac surgery by 600 interventions. This means 600 critical patients less in the waiting list. With 38m €, the number of cardiac interventions would be 2.280.Ask yourself what to do about it, what would you prefer to do with 38m€ every year ? Just apply them to 249 patients or to 2.280 (you are not on the waiting list, and we'll assume the same adjusted quality of life years for both cases). Anyway, it's too late to have your answer, the government has already decided for you, and maybe you don't agree with it, as I don't agree. The government prefers the rescue of 249 citizens.
Just to finish, check this final fact:
This country spends 1.192 € per capita of public budget on health. Another country under the same mandatory tax system is able to spend 1.635 €, 40% more !!!More money allows to avoid such dilemmas for this country. Ask yourself if you want to stay in the former tax system that is damaging your health. Once you have the answer, you'll understand why this country wants to leave this unfair tax system as soon as possible.
Subscriure's a:
Missatges (Atom)