Design of financial incentives and payment schemes in healthcare systems: A review
27 de març 2021
26 de març 2021
What the hell do these people actually mean by "value" in healthcare?
On the Much Used (and Abused) Word "Value" in Healthcare
A must read speech by Uwe Reinhardt (RIP). Selected statements:
Now, when I listen to all this prattle on value among people of the real world, I ask myself, what the hell do these people actually mean by that? Well, you typically find it defined as outcomes relative to cost, and then encompassing efficiency. Now, you can have fun with this expression in New England as I had, there were all providers, they were all from the supply side and I said, “It’s a great expression, I never thought of it as an economist but let me play with it. See what you can do with this.” So let’s look at this equation. The first thing you’ll know is that quality is multi-dimensional, it’s a vector. We geeks, have a certain aversion to dividing a vector by a dollar figure. Somehow it is hard to teach this, so we invented this little magic machine that can mush up vectors of quality with vectors of utility, feelings, and out comes this thing called a “qaly” (quality adjusted live year). And you know, Bismarck says you should never inquire how laws are made it’s like making sausages. This is worse, this is actually a little bit like making dog food, but you know earnings per share on an income statement is worse in terms of its reliabilities. So let us look at this ratio where we have value equalling qaly over cost, which, by the way, the inverse of that is just what we call cost effectiveness.
The more you think about this ratio, you run into a very famous law, Alfred E. Newman’s. Now, who in this audience knows Alfred E. Newman? You’re the most educated. You know kids nowadays don’t know anything, no wonder they’re so weird. They’re not well-read. We all grew up on Mad Magazine which kept us sane. If you hadn’t read Mad Magazine you’d all be nuts by now because Alfred E. Newman understood the world. Here is this famous law, one person’s healthcare cost is another ones healthcare income. Now that’s worth a Nobel laureate. So following Alfred E. Newman’s law, I’m going to write it like this and you can do that to healthcare providers and you see their little eyes ask, could this be true? Who here has ever served on a hospital board? I have on both for profit and not for profit. At any health clinic, what do they talk about: growth, growth, growth. It means revenue, so they don’t want to hear this. They want more qalys and more revenue, that’s what they really want. So, ask yourself this question; has anyone ever thought that the supply side folks want to create value for the patient by cutting their own revenue? I’ve never heard of that.
Imagine a hospital board with an agenda item: 30 minutes on enhancing value for patients by lowering our revenue. Not thinkable. Has anyone ever seen such a board, or even an agenda item? I have served for over a decade on these boards, and not once. You know growth usually gets an hour; patient safety now gets a half hour. But efficiency, not once have I ever heard of it. It gets worse. We have this equation: revenue equals price times quantity times volume. Can you imagine how obscene that is to a hospital executive? Because they ask, “You mean we can create value by cutting prices? Aren’t prices and quality positively correlated?” And you say, “Why would you say that?” Even if you’re drunk, why would you ever say that? You know, so the hospital raises its price and you get more value.
Highly recommended!
25 de març 2021
COVID persistent public health policies
Policy responses need to take account of the complexity of Long COVID and how what is known about it is evolving rapidly. Areas to address include:
– The need for multidisciplinary, multispecialty approaches to assessment and management;
– Development, in association with patients and their families, of new care pathways and contextually appropriate guidelines for health professionals, especially in primary care to enable case management to be tailored to the manifestations of disease and involvement of different organ systems;
– The creation of appropriate services, including rehabilitation and online support tools;
– Action to tackle the wider consequences of Long COVID, including attention to employment rights, sick pay policies, and access to benefit and disability benefit packages;
– Involving patients both to foster self-care and self-help and in shaping awareness of Long COVID and the service (and research) needs it generates; and
– Implementing well-functioning patient registers and other surveillance systems; creating cohorts of patients; and following up those affected as a means to support the research which is so critical to understanding and treating Long COVID.
24 de març 2021
The risks of unregulated genomics
Regulating the unknown. A guide to regulating genomics for health policy-makers
In the absence of appropriate regulation and guidance, the exceptionally detailed type of information on individuals that is generated by genomics may pose a threat to privacy and undermine the concept of risk pooling and the values of universality, equity and solidarity that underpin European health systems by turning potential risks for everyone into likelihoods for a few.
This policy brief provides some hint for effective regulation of genomics and describes the current initiatives. A good summary.
23 de març 2021
Risk-adjusted cost-effectiveness
Cost-effectiveness analysis (CEA) embeds an assumption at odds with most economic analysis–that of constant returns to health in the creation of happiness (utility). We aim to reconcile it with the bulk of economic theory.
Therefore,
As health payers increasingly turn to CEA for value assessment, it becomes even more important to assure that it reflect the preferences of real people. Current models run an important risk by not considering the consequences of diminishing returns and risk aversion over health. Continuing to assume that the incremental value of health is invariant to severity of illness endangers the foundations of CEA. The combination of the diminishing returns and severity of illness adjustments suggests that we are probably overvaluing treatments of low-severity illnesses (possibly by a factor of 2 or more) and undervaluing treatments of very high-severity conditions (possibly by a factor of 5 or more).
This is solved by the GRACE framework that shows how to generalize traditional CEA models to incorporate the effects of diminishing returns to health improvements as severity of illness increases. This creates cost-effectiveness thresholds (stated as multipliers of consumption) that incorporate risk preferences both in consumption and in QoL and that increase with severity of illness.
22 de març 2021
Value based health care
Building on value-based health care
A reminder:
Within the context of solidarity-based European health care systems and the mounting concerns about ensuring financial sustainability of universal health care, the European Commission Expert Panel on
Effective Ways in Investing in Health (EXPH) [3] proposed a comprehensive concept of value-based health care based on four pillars of value:
• achievement of best possible outcomes with available resources (technical value);
• equitable distribution of resources across all patient groups (allocative value);
• appropriate care to achieve each patient’s personal goals (personal value);
• contribution of health care to social participation and connectedness (societal value).
Examples of value-based health care initiatives identified by the EXPH that can contribute to more effective, accessible and resilient health care systems include: reallocation of resources through disinvestment for reinvestment; addressing unwarranted variation, defined as variation in the utilization of health care services that cannot be explained; fighting corruption, fraud and misuse of public resources; increasing public value in biomedical and health research; regulatory policies aimed at improving access to high-value (but costly) medicines; incentives for fairer distribution; and more optimal use of resources.
A well known approach, opposite to creating value through market competition (Porter style).
21 de març 2021
A value framework for diagnostic tests
Useful article, beyond the title, you'll find different value frameworks to apply to diagnostic tests and their proposal:
Table 4. Value framework proposed.
| Essential/core | |
| Criteria∗ | Subcriteria∗ |
| Clinical Benefit and Test Performance | Clinical consecuences of the use of the test |
| Test performance | |
| Safety and Unwanted consequences | Procedural safety |
| Consequences of the wrong diagnosis | |
| Safety of test preparation | |
| Safety of test operators | |
| Quality of scientific evidence | |
| Economical aspects | Economic evaluation (clinical effectiveness and/or budget impact analysis) |
| Other costs | |
| Organizational aspects and feasibility within the clinical path | Impact on the health services provision system |
| Impact on the path of patient care | |
| High importance | |
| Health priority of the health system | |
| Disease burden | |
| Equity | Neglected diseases test |
| Test in communicable diseases and high prevalence | |
| Low access to health services | |
| Ethical and legal aspect | |
| Severity of the disease | |
| Absence of alternative diagnostic technologies | |
| Medium importance | |
| Nonclinical benefits | Experience of who takes the test |
| Value of the information | |
| Load on caregivers or family | |
| Preparation and/or care | |
| Number of results associated with the test | |
| Test processing time | |
| Self test | |
| Environmental impact | |
| Broader social impact | |
| Low importance | |
| Innovation | |
- ∗
See definitions of criteria and subcriteria in Appendix 3 (in Supplemental Materials found at https://doi.org/10.1016/j.jval.2020.11.008).
20 de març 2021
Distributional cost-effectiveness
Distributional Cost-Effectiveness Analysis. Quantifying Health Equity Impacts and Trade-Offs
Distributional Cost-Effectiveness Analysis Comes of Age
Distributional cost-effectiveness analysis (DCEA) provides information about the equity impacts of health technologies and programs and the trade-offs that sometimes arise between equity and efficiency. This field has now come of age with a growing applied literature,1 new training resources,2 and a formal professional network: a special interest group on equity-informative economic evaluation within the International Health Economics Association
The outline of the book:
Part One: Preliminaries
1:Introduction, Richard Cookson, Susan Griffin, Ole F. Norheim, Anthony J. Culyer
2:Principles of health equity, Richard Cookson, Anthony Culyer, Ole F. Norheim
3:Designing a distributional cost-effectiveness analysis, Richard Cookson, Susan Griffin, Ole F. Norheim, Anthony J. Culyer
4:Describing equity impacts and trade-offs, Richard Cookson, Susan Griffin, Ole F. Norheim, Anthony J. Culyer
5:Introduction to the training exercises, Richard Cookson, James Love-Koh, Colin Angus, James Lomas
Part Two: Simulating Distributions
6:Health by disease categories, Kjell Arne Johansson, Matthew M. Coates, Jan-Magnus Økland, Aki Tsuchiya, Gene Bukhman, Ole F. Norheim, Øystein Haaland
7:Health by social variables, James Love-Koh and Andrew Mirelman
8:Costs and health effects, Colin Angus
9:Health opportunity costs, James Love-Koh
10:Financial protection, Andrew Mirelman and Richard Cookson
Part Three: Evaluating Distributions
11:Dominance analysis, Owen O'Donnell and Tom Van Ourti
12:Rank-dependent equity weights, Owen O'Donnell and Tom Van Ourti
13:Level-dependent equity weights, Ole F. Norheim, Miqdad Asaria, Kjell Arne Johansson, Trygve Ottersen and Aki Tsuchiya
14:Direct equity weights, Mike Paulden, James O'Mahony and Jeff Round
Part Four: Next Steps
15:Uncertainty about facts and heterogeneity of values, Susan Griffin
16:Future challenges, Richard Cookson, Alec Morton, Erik Schokkaert, Gabriela B. Gomez, Maria Merritt, Ole F. Norheim, Susan Griffin, and Anthony J. Culyer
19 de març 2021
The business of vaccines
Covid-19 and the business of vaccines
The FT explains the business models behind vaccines and asks if the Covid-19 pandemic will fundamentally change the vaccine market. This short documentary features global experts including Bill Gates, the CEOs of Moderna and Gavi, and the lead scientist behind the Oxford/AstraZeneca vaccine
18 de març 2021
The low marginal benefit of ultra-expensive drugs
Assessing the Added Therapeutic Benefit of Ultra-Expensive Drugs
In US:
The number of ultra-expensive drugs and Medicare beneficiaries taking these drugs has grown significantly, resulting in a very high concentration of Medicare Part D spending on ultraexpensive drugs. Between 73% and 85% of these drugs assessed in France, Canada, or Germany received a low added therapeutic benefit rating. Policy reforms to address drug prices in the United States should consider developing an assessment framework for added therapeutic benefit to incentivize and reward the development of drugs that offer a significant clinical improvement over the current standard of care. In the interim, use of international assessments would be possible.
However, it may seem weird to our eyes, but:
Medicare Part D in particular has a problem with ultra-expensive drugs, since it pays nearly 80% of the cost of these drugs, and by law Medicare cannot directly negotiate the price for these drugs with the drug companies
Public funding without the possibility to set the contract for low marginal benefit drugs! The result:
Medicare Part D spending on brand-name drugs for these ultra-expensive drugs increased from 1.5% in 2012 to 19% in 2018
The answer is change the law and set benefits package according to added value.
17 de març 2021
The long and bumpy road to CRISPR (3)
CRISPR People. The Science and Ethics of Editing Humans
A book on the ethics of CRISPR, without a clear prescription, only a review of He horrendous experiment and a personal view of the current situation.
This has been a cautionary tale about scienceand scientists. People can overreach. He Jiankui, driven as far as I can tell by what Macbeth called “vaulting ambition, which o’erleaps itself,”1 and aided by a serious lack of scruples, behaved terribly. He put three lives at needless and reckless risk (and tried to do the same to more). The story is also a cautionary tale for Science. He Jiankui damaged Science by reinforcing the Victor Frankenstein image—the mad, uncontrolled scientist. Most scientists, and hence most science, are much more rule bound, constrained by the needs of getting and keeping jobs, tenure, and most importantly grants, as well as wrapped, in most countries, in many bureaucratic threads of control. But He happened, and Science needs both to act to minimize the harm he has caused and to be seen to be doing so.
A global consensus is a chimera. Seven and a half billion people are not going to agree on this issue—nor will the fraction of those who understand it. Neither will the roughly 200 countries of the world, at least at anything other than a lowest common denominator. Not all countries have agreed to various nuclear weapons or climate change treaties in spite of the apparently obvious need for them. If somehow something close to unanimity were achieved, it would probably be at the cost of precision. Thus, the Council of Europe enacted a convention that banned human cloning, but effectively left open the then-hot question whether it covered just reproductive cloning or “research cloning” (of human embryos for only ex vivo use) by not defining a “human being.” It also left the implantation and enforcement of such a ban up to the member nations, some of whom were probably happy, for political reasons, to sign it but will have little interest in enforcing it.
And this is the controversial position of the author:
One might argue that human germline genome changes are irreversible, or less reversible, than some other interventions. But is that true? A mistaken genome change could presumably be reedited, in a living person or in that person’s germline (or embryos), to reverse the error. Or it could be selected against in the individual’s offspring, through PGD or otherwise. It could be too late to avoid harm to the edited person, but that mistake will not have to pass on from generation to generation. Human germline genome editing does raise important questions about safety, coercion, equity, diversity, and enhancement. These are not unique to editing the human germline genome. They also apply to somatic cell DNA editing, to new drugs, to smartphones, to climate change, and to many other changes from technologies. Questions about reversibility also apply; the social effects of cell phones are probably less reversible than genome edits. The fact that a technological change is in “the human germline genome” should have no special ethical weight.
Really? Security in CRISPR is not unique???
16 de març 2021
Changing the production function of diagnostic tests (2)
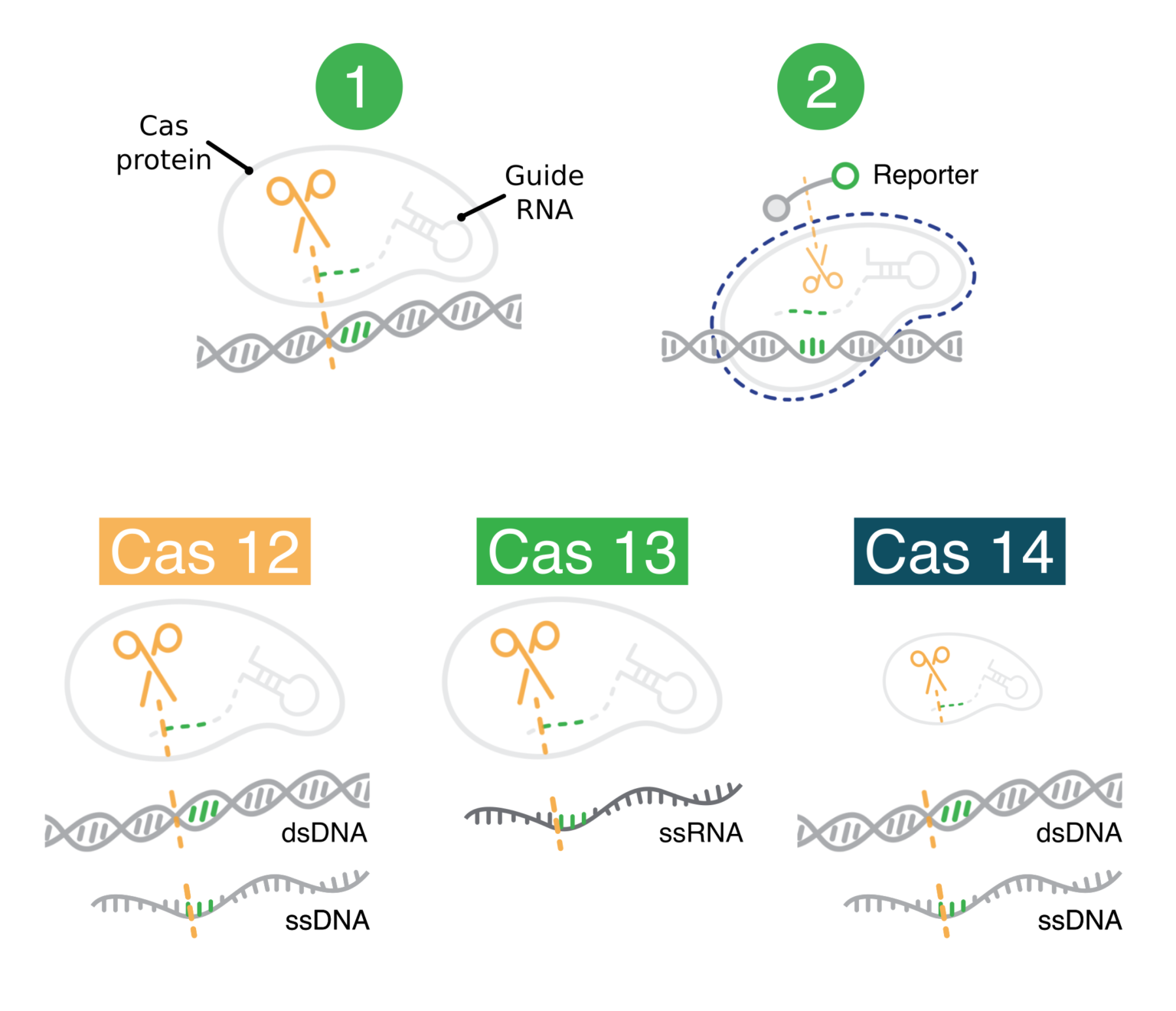
The Cas proteins behind CRISPR diagnostics
CRISPR diagnostics explained in few words:
There are many protein tools in the CRISPR toolbox. Each is suited to a particular suite of uses. For example, the common CRISPR protein Cas9 is well suited for genome editing. It is not suited for CRISPR diagnostics. In this blog post, we’ll introduce you to the proteins behind CRISPR diagnostics: Cas12, Cas13, and Cas14.
CRISPR diagnostics have two key components:
- Protein-guide molecule complexes. These first cut specific nucleic acid sequences that the user wants to detect. After cutting a user-specified sequence, these complexes non-specifically cut other nucleic acids.
- Modified nucleic acids (reporters). These produce a visual signal when cut. They are only cut if the user-specified nucleic acids are cut first. These modified nucleic acids make it easy to observe when the user-specified nucleic acids have been detected (cut).
15 de març 2021
COVID epistemology
Why Does the Pandemic Seem to Be Hitting Some Countries Harder Than Others?
And there lies an epidemiological mystery. The usual trend of death from infectious diseases—malaria, typhoid, diphtheria, H.I.V.—follows a dismal pattern. Lower-income countries are hardest hit, with high-income countries the least affected. But if you look at the pattern of covid-19 deaths reported per capita—deaths, not infections—Belgium, Italy, Spain, the United States, and the United Kingdom are among the worst off.
This is the unfixed conundrum explained by Siddhartha Mukherjee in The New Yorker, And no clear answer, you may read the whole article to confirm it.
The covid-19 pandemic will teach us many lessons—about virological surveillance, immunology, vaccine development, and social policy, among other topics. One of the lessons concerns not just epidemiology but also epistemology: the theory of how we know what we know. Epidemiology isn’t physics. Human bodies are not Newtonian bodies. When it comes to a crisis that combines social and biological forces, we’ll do well to acknowledge the causal patchwork. What’s needed isn’t Ockham’s razor but Ockham’s quilt.
Above all, what’s needed is humility in the face of an intricately evolving body of evidence. The pandemic could well drift or shift into something that defies our best efforts to model and characterize it.
Great documentary, on Knoedle gallery fake art
14 de març 2021
CRISPR: from lab to the clinic
This is the year that CRISPR moves from lab to clinic
Jennifer Doudna says:
In 2021, researchers will use CRISPR to enhance our medical response to the Covid-19 pandemic. Teams will continue to collaborate and bring to market vital CRISPR-based diagnostic tools that are accurate, rapid and painless. One currently being developed and scaled by Mammoth Biosciences, a company I co-founded, along with partners at the University of California, San Francisco and the pharmaceutical company GSK, can detect and indicate the presence of SARS-CoV-2 RNA in a similar fashion to a pregnancy test.
CRISPR will also have an important effect on the way we treat other diseases. In 2021, we will see increased use of CRISPR-Cas enzymes to underpin a new generation of cost-effective, individualised therapies. With CRISPR enzymes, we can cut DNA at precise locations, using specifically designed proteins, and insert or delete pieces of DNA to correct mutations.
This is precisely what is going on.