Explainable AI in Healthcare. Unboxing Machine Learning for Biomedicine
Solving the explainable AI conundrum by bridging clinicians’ needs and developers’ goals
Tot això va molt ràpid. I potser algú s'hauria de posar a revisar-ne els fonaments i les seves conseqüències. Em refereixo en concret al que es coneix com explicabilitat de la intel·ligència artificial. En aquest blog m'hi he referit com Black Box Medicine.
Caldria que els algoritmes que s'utilitzen puguin ser permeables al coneixement dels humans, o dit altrament, que si no és explicable doncs aleshores no sabem com s'arriba al resultat i que si ho repliquem tampoc sabem si sortirà el mateix (fiabilitat). A les ciències de la vida és encara més rellevant, perquè l'impacte pot ser determinant per la salut i la vida.
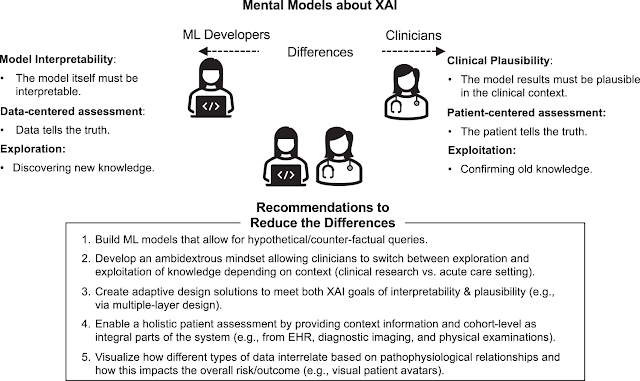
Avui aporto un llibre i un article. El llibre no l'he llegit, però tinc la impressió que és el més complet que hi ha per ara en aquesta qüestió des d'un punt de vista pràctic. L'article de Nature reflecteix les perspectives dels informàtics versus els clínics, i en una gràfica es mostra tot:
I ja podem veure que no hi ha acord i que cal reduir les diferències de perspectiva. Per ara ha sortit guanyant els primers.
Del llibre en reprodueixo l'índex:
1. Human–AI Relationship in Healthcare
2. Deep Learning in Medical Image Analysis: Recent Models and Explainability
3. An Overview of Functional Near-Infrared Spectroscopy and Explainable Artificial Intelligence in fNIRS
4. An Explainable Method for Image Registration with Applications in Medical Imaging
5. State-of-the-Art Deep Learning Method and Its Explainability for Computerized Tomography Image Segmentation
6. Interpretability of Segmentation and Overall Survival for Brain Tumors
7. Identification of MR Image Biomarkers in Brain Tumor Patients Using Machine Learning and Radiomics Features
8. Explainable Artificial Intelligence in Breast Cancer Identification
9. Interpretability of Self-Supervised Learning for Breast Cancer Image Analysis
10. Predictive Analytics in Hospital Readmission for Diabetes Risk Patients
11. Continuous Blood Glucose Monitoring Using Explainable AI Techniques
12. Decision Support System for Facial Emotion-Based Progression Detection of Parkinson’s Patients
13. Interpretable Machine Learning in Athletics for Injury Risk Prediction
14. Federated Learning and Explainable AI in Healthcare
Si un dels principis de la bioètica com diu Floridi, hauria de ser l'explicabilitat, ens queda un llarg camí per aconseguir que així sigui. Tinc la impressió que estem davant una estratègia de fets consumats: els algoritmes són aquí, i no sé explicar com s'arriba a aquest resultat amb aquest algoritme.
PS. Ha arribat la intel·ligència artificial open source, la regulació i explicabilitat esdevenen encara més rellevants.